Introduction
Navigating the complexities of a claims denial letter can often feel overwhelming. We understand that many individuals are left unsure of their next steps. However, grasping the nuances of the denial notice is crucial; it can significantly influence the outcome of your appeal.
This guide delves into essential strategies for effectively contesting a denial. We’ll address common pitfalls and empower you to reclaim your rights. How can you transform a frustrating rejection into a successful appeal? What vital steps must you take to ensure a smooth process?
You are not alone in this journey. Together, we can explore the path to a successful appeal.
Understand the Denial Letter's Content and Implications
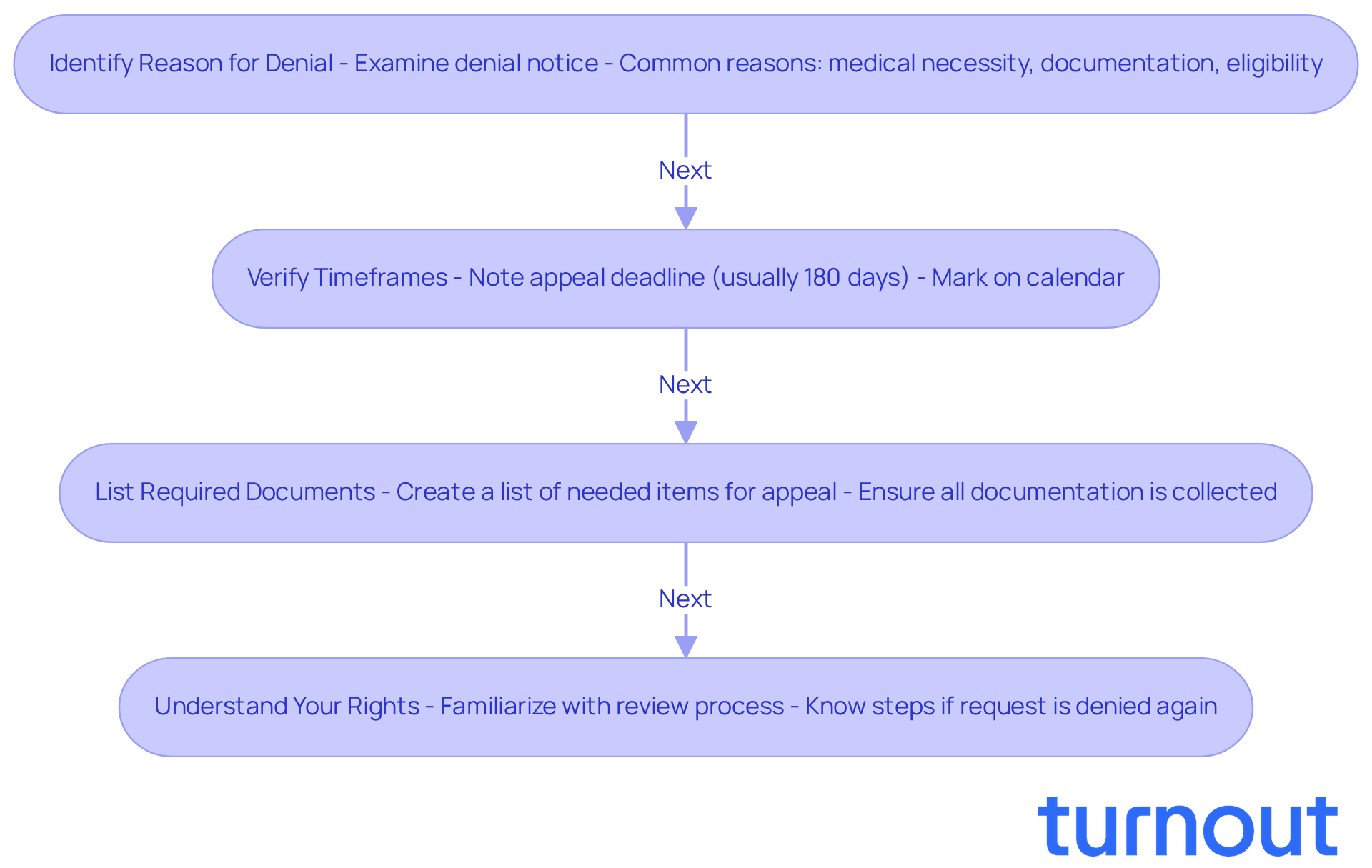
To effectively contest a claims denial letter, it’s important to start by carefully examining the denial notice. We understand that this can be a frustrating experience, but breaking it down can help you navigate the process more easily:
-
Identify the Reason for Denial: Pay close attention to the specific language used in the letter. Common reasons that result in a claims denial letter include lack of medical necessity, insufficient documentation, or failure to meet eligibility criteria. Understanding these reasons is essential, as they will guide your strategy for requests. Research shows that about 10% of health insurance claims submitted are rejected, so addressing these reasons directly in your request is crucial.
-
Verify Timeframes: Most rejection notifications outline a period during which you need to submit your challenge, usually 180 days from the date of refusal. Mark this date on your calendar to ensure you don’t miss it. Missing the deadline may require you to start a new application, which could result in losing the original filing date and potential back payments.
-
The claims denial letter may specify what additional information or documents are needed for your appeal. Create a thorough list of these items to ensure you collect everything required. Inadequate records are a common cause for initial denials, and many applicants fail to provide sufficient documentation, which can significantly hinder their chances of success.
-
Understand Your Rights: Familiarize yourself with your entitlements regarding the review process. This includes knowing that you can request a review of the decision and understanding the steps to follow if your request is denied again. Being aware of your rights can empower you to navigate the review system effectively. Consumer advocates emphasize the importance of examining rejection notices to ensure you are fully aware of your options.
By comprehending the claims denial letter, you can approach your request with clarity and purpose, significantly enhancing your chances of achieving a favorable result. Research indicates that requests are more likely to succeed when applicants fully understand the reasons for rejection and address them directly in their submissions. Remember, you’re not alone in this journey; we’re here to help.
Gather Necessary Documentation and Evidence for Your Appeal
If you've received a claims denial letter regarding your insurance claim, know that you're not alone. It’s crucial to gather the right evidence to support your case. Here’s how you can navigate this process with confidence:
-
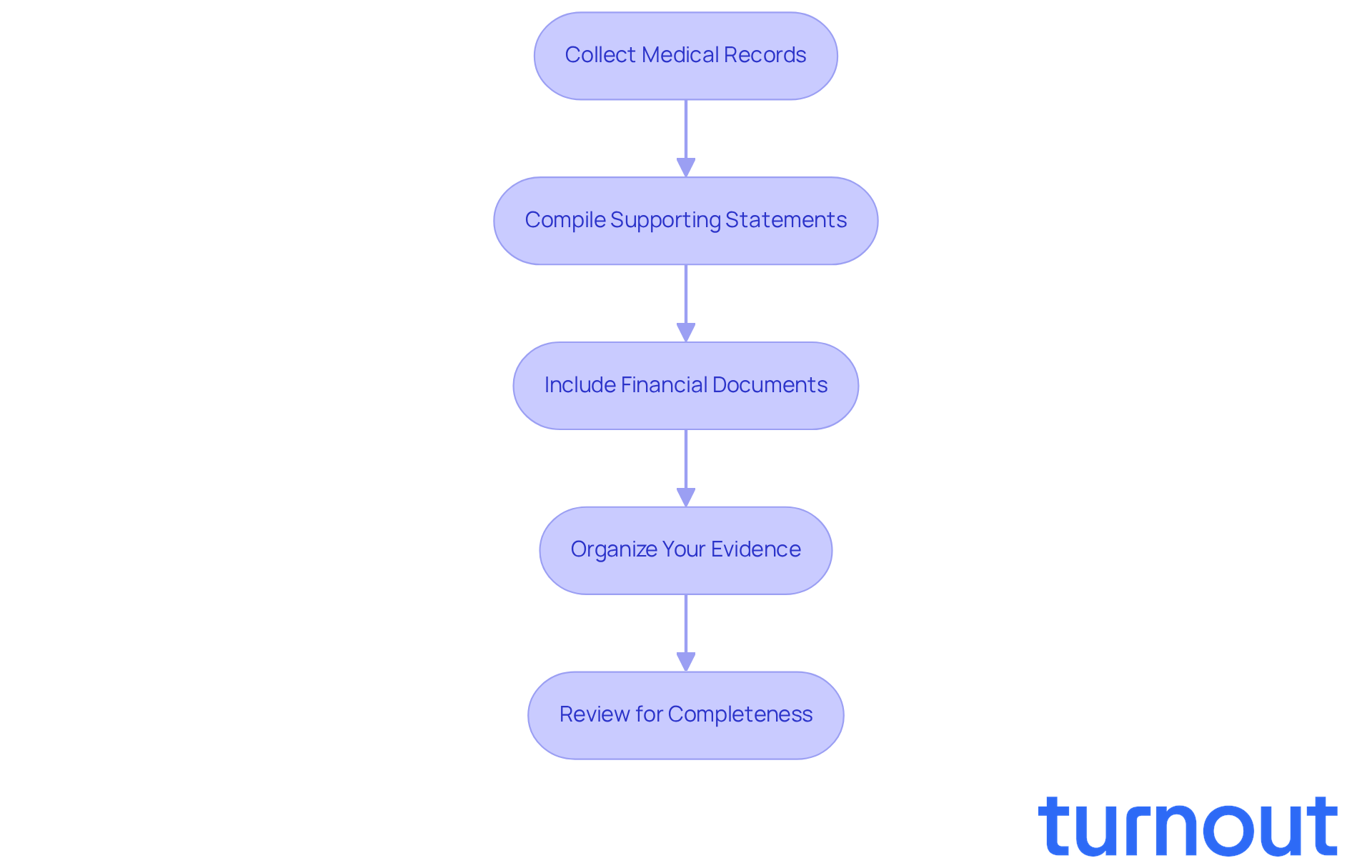
Collect Medical Records: Start by securing all relevant medical records that back up your claim. This includes doctor’s notes, treatment plans, and test results that clearly outline your condition and treatment history. Strong documentation is vital. Studies show that patients who challenge their denials often succeed, especially when they have comprehensive medical records. In fact, those who appealed claim denials were winning about half the time.
-
Compile Supporting Statements: If you can, obtain statements from healthcare providers that affirm your condition and the necessity of the denied services or benefits. These endorsements can significantly strengthen your case. Healthcare professionals emphasize the importance of clear communication regarding medical necessity, and having robust documentation is essential for a successful challenge.
-
Include Financial Documents: If your request involves financial assistance or benefits, be sure to include any relevant financial documents that illustrate your need for support. This can help convey the urgency of your situation and the impact of the rejection on your financial well-being.
-
Organize Your Evidence: Create a well-organized folder, whether physical or digital, to keep all your documents in order. Clearly label each document and maintain a checklist to ensure nothing is overlooked. Proper organization can make the submission process smoother and reduce the chances of errors.
-
Review for Completeness: Before you submit your request, take the time to meticulously review all documents. Confirm that you’ve included everything specified in the claims denial letter. Incomplete submissions can lead to further delays or additional denials, so thoroughness is key.
If you find yourself needing assistance with the appeals process, consider reaching out to the Patient Advocate Foundation. They offer complimentary case management services for complicated cases.
By gathering thorough records, you not only enhance your request but also lay a strong foundation for your case, increasing your chances of a favorable outcome. Remember, we're here to help you through this journey.
Draft a Strong Appeal Letter Addressing Key Concerns
With your documentation in hand, it’s time to compose your request. Here’s how to create a compelling letter:
-
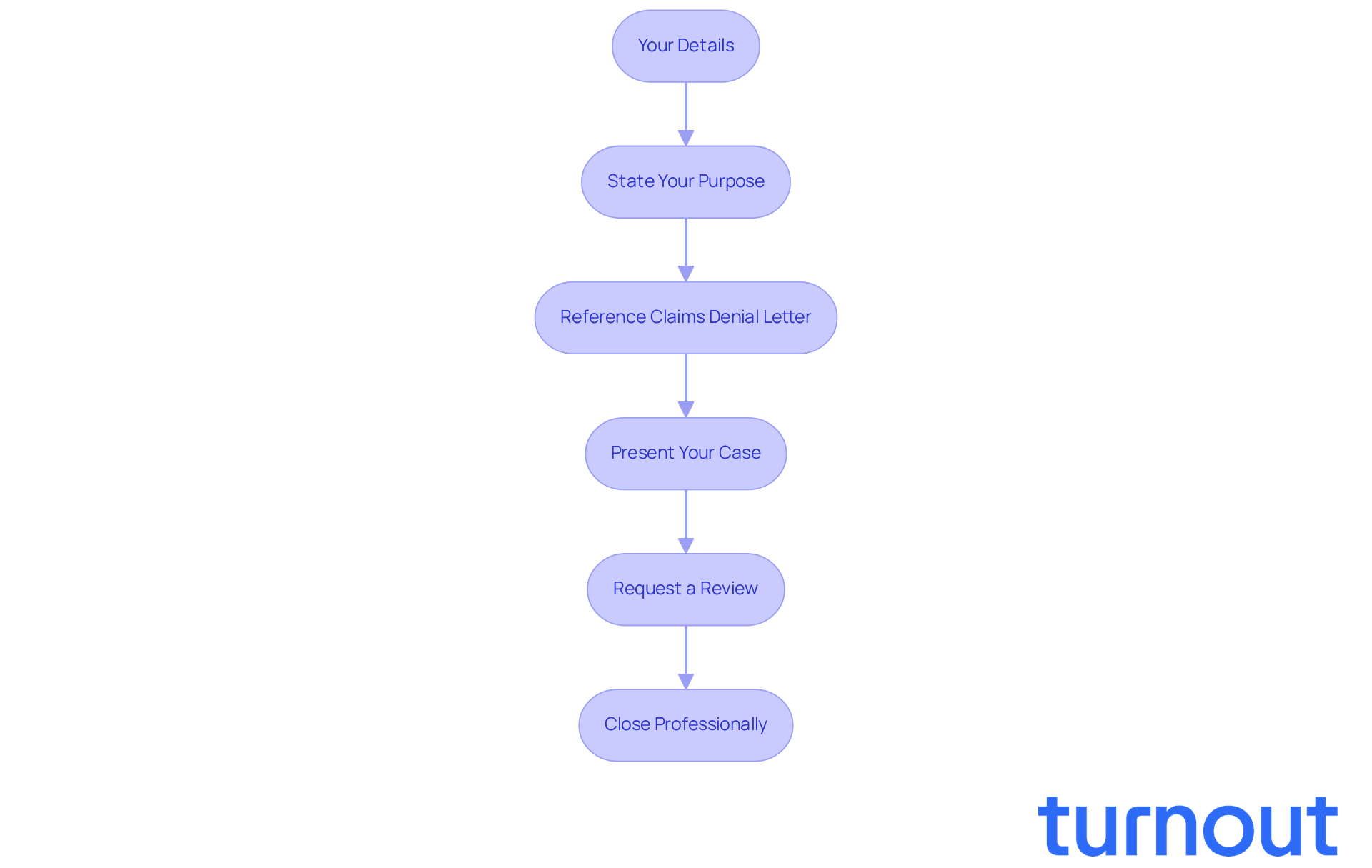
Begin with Your Details: Start by including your name, address, and contact information at the top of the document. Don’t forget to add the date and the insurance company’s address.
-
State Your Purpose: Open your letter with a clear declaration of your intent to contest the rejection. For example, you might say, "I am writing to officially contest the rejection of my claim dated [insert date]." This sets the tone for your appeal.
-
Reference the claims denial letter: It’s important to mention the specific claims denial letter you received, including the date and the reason for the refusal. This helps the reviewer quickly locate your case and understand the context of your appeal.
-
Present Your Case: Clearly outline why you believe the refusal was incorrect. Use the materials you collected to support your assertions. Stick to the facts and avoid emotional language. Highlight any common mistakes that may have led to the denial, such as incomplete medical documentation or failure to follow prescribed treatments, which often account for a significant percentage of initial denials.
-
Request a Review: Politely ask the insurance company to review your case and reconsider their decision based on the new evidence you’ve provided. Remember, many successful appeals stem from well-documented cases. Thousands of applicants obtain benefits each year through persistent efforts, and you can be one of them.
-
Close Professionally: Conclude your letter with a formal closing, including your signature and printed name. Consider sending the document via certified mail to ensure it is received and recorded.
By following these steps, you can create a powerful request letter that effectively communicates your case. Remember, representation by seasoned advocates can greatly enhance your likelihood of success. They understand the intricacies of the process and can assist you in navigating it more efficiently. You are not alone in this journey.
Follow Up on Your Appeal Submission and Stay Informed
After submitting your request, it’s important to stay informed about its progress. We understand that this can be a stressful time, so here’s how to effectively follow up:
-
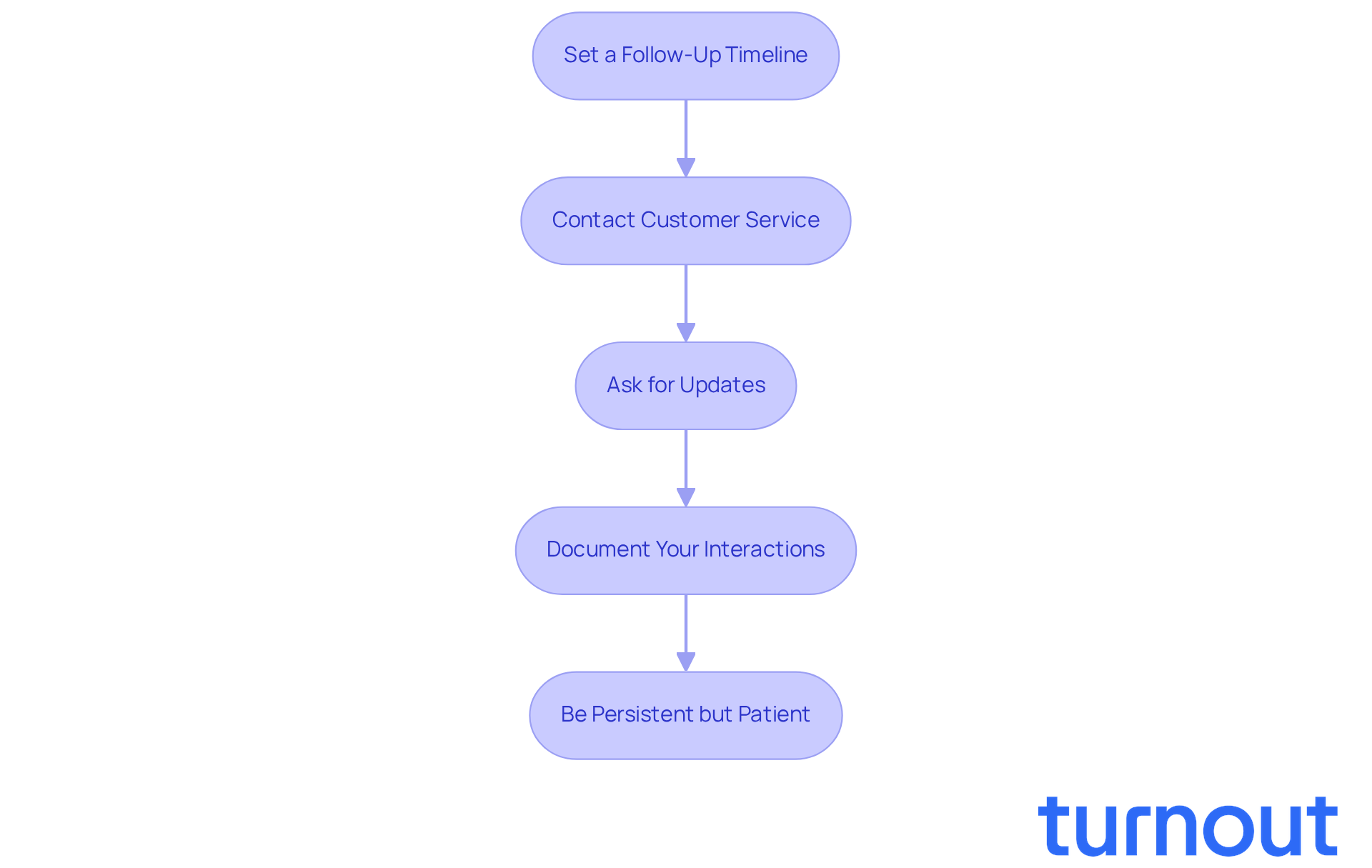
Set a Follow-Up Timeline: Schedule a follow-up for 1-2 weeks after submission. This gives the insurance company enough time to handle your request.
-
Contact Customer Service: Reach out to the customer service number provided in the rejection letter or on the insurer's website. Have your claim number and personal details ready for verification. This step can feel daunting, but it’s essential for clarity.
-
Ask for Updates: Inquire about your appeal's status and whether any additional information is needed. This proactive approach not only helps expedite the process but also shows your commitment to resolving the issue. Remember, many insurance rejections occur because AI systems dismiss claims without human evaluation, so staying involved is crucial.
-
Document Your Interactions: Keep detailed records of all communications, including dates, times, and the names of representatives you speak with. This documentation is invaluable if further complications arise. Additionally, gather all reference numbers mentioned in the claims denial letter, as they are necessary for future interactions with insurance representatives.
-
Be Persistent but Patient: While following up is essential, patience is equally important. Appeals can take time, and being overly aggressive may hinder your progress. It’s common to feel frustrated, but statistics show that nearly 40% of patients who appeal a second or third time win their claims. This highlights the importance of persistence. By diligently following up and ensuring comprehensive documentation, you can address any potential issues before they escalate. Remember, you are not alone in this journey; we’re here to help.
Conclusion
Navigating the complexities of a claims denial letter can feel overwhelming, but it doesn’t have to be. We understand that facing a denial can be disheartening. However, by grasping the contents and implications of the denial, gathering the necessary documentation, drafting a strong appeal letter, and following up diligently, you can significantly improve your chances of a successful appeal. This structured approach empowers you to tackle the appeals process with confidence and clarity.
Key insights from this article highlight the importance of:
- Identifying the reason for denial
- Verifying timeframes
- Ensuring that all required documentation is complete and well-organized
By addressing the specific concerns outlined in the denial letter and presenting a compelling case, you can effectively advocate for your rights and potentially overturn unfavorable decisions. Remember, persistence, patience, and thoroughness are essential components of this journey.
Ultimately, appealing a claims denial is not just about the immediate outcome; it’s about understanding your rights and navigating the system with determination. Whether it’s reaching out for assistance or following up on the status of your appeal, staying informed and proactive can make a significant difference. Embracing these steps can lead to not only a successful appeal but also a more empowered approach to managing health insurance claims in the future. You're not alone in this journey, and we're here to help.




