Introduction
Navigating the murky waters of insurance denial letters can feel overwhelming. We understand that this experience often leaves individuals frustrated and unsure of their next steps. These letters contain crucial information that can help you dispute a denial and reclaim the benefits you deserve.
But what if the denial seems unjustified? What if the path to appeal feels unclear? You're not alone in this journey. This article will guide you through essential steps to master your response. Together, we can transform a setback into a triumph in your insurance journey.
Review the Denial Letter Thoroughly
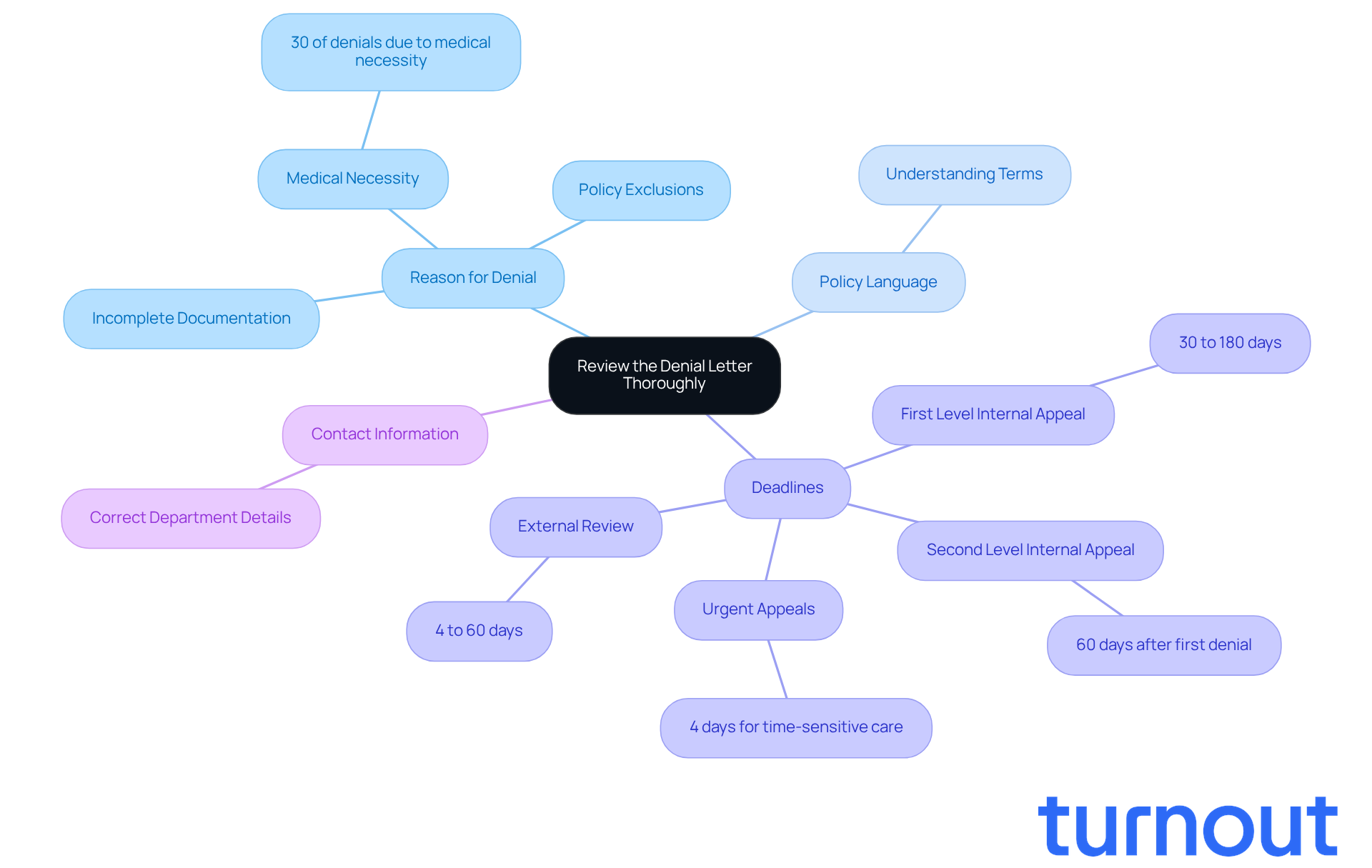
Begin by carefully reviewing the insurance denial letter you received from your insurance company. We understand that this can be a frustrating experience, so let’s break it down together. Pay close attention to these key components:
- Reason for Denial: Clearly identify the specific reasons your claim was denied. Common issues include lack of medical necessity, policy exclusions, or incomplete documentation. Notably, Cigna HealthCare of North Carolina indicated that 30% of rejection reasons were due to medical necessity. This highlights how crucial thorough documentation is in your case.
- Policy Language: Take note of any references to policy language that the insurer cites as justification for the denial. Understanding these terms is essential for crafting a persuasive request.
- Deadlines: Look for any deadlines mentioned for submitting a request. Most insurers require requests for reconsideration to be submitted within a specific timeframe, typically ranging from 30 to 180 days depending on the plan. Missing these deadlines is a common reason for claim denials, so it’s vital to act promptly.
- Contact Information: Ensure you have the correct contact details for the department managing requests. This will be necessary for your next steps.
By understanding these elements, you can effectively prepare for your request and directly address the insurer's concerns, increasing your chances of a successful outcome. As public adjuster Scott Friedson highlights, 'Missed deadlines are a top reason for rejection.' Staying organized and proactive is essential. Additionally, for urgent situations, be aware that expedited appeals can be reviewed in as little as 72 hours. Remember, understanding the insurance denial letter is the first step in transforming a setback into a success. You are not alone in this journey; we’re here to help.
Dispute the Denial with Strong Evidence
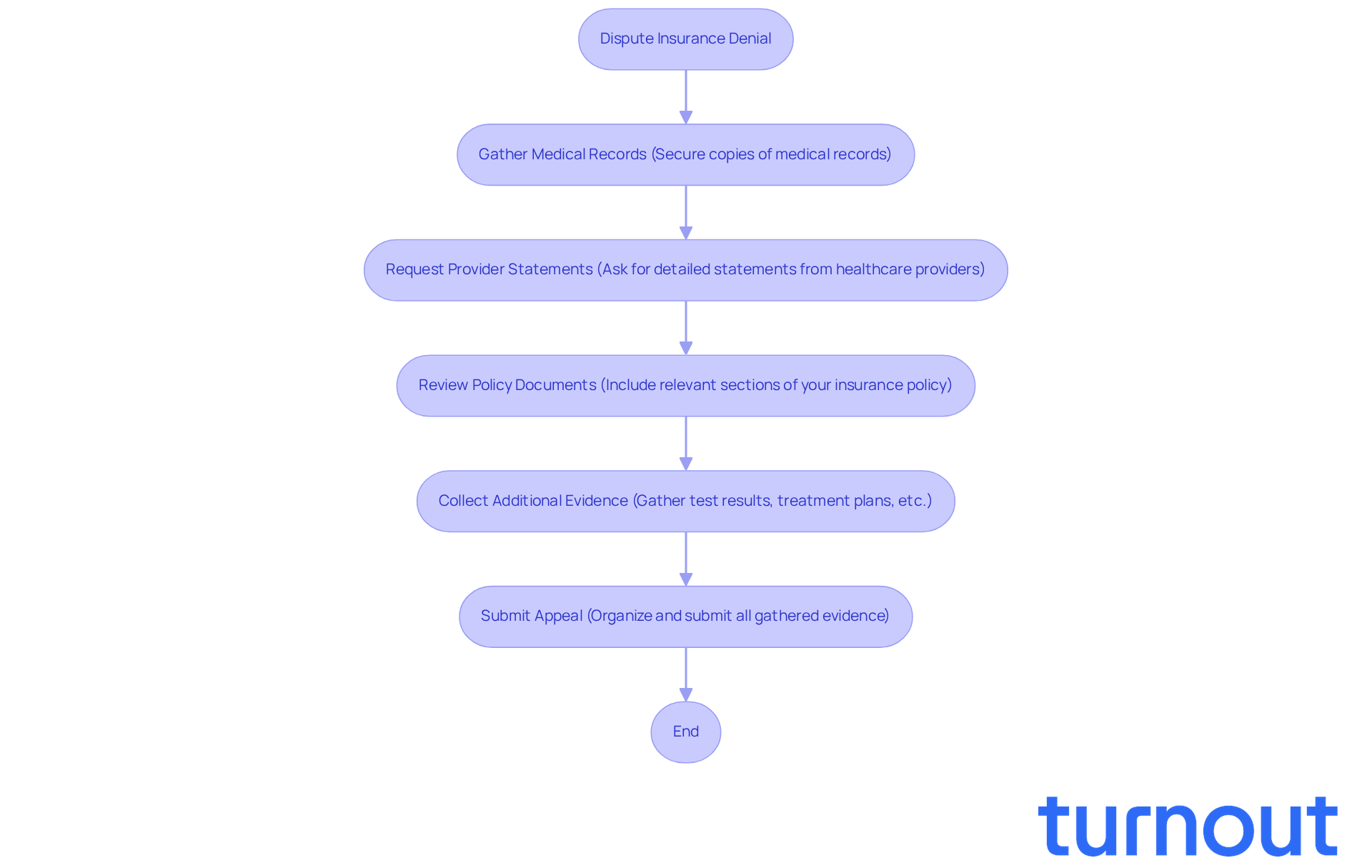
Disputing an insurance denial letter can feel overwhelming, but you’re not alone in this journey. To effectively challenge a denial, start by gathering all the necessary documentation to support your case. Here’s how:
- Medical Records: Make sure to secure copies of your medical records that clearly show why the denied treatment or service was necessary. Comprehensive documentation is crucial. Studies reveal that requests backed by thorough medical records have a much higher success rate. In fact, patients who carefully follow the reconsideration process can join the 80% who successfully overturn denied claims.
- Provider Statements: Don’t hesitate to ask your healthcare provider for a detailed statement that explains the medical necessity of the treatment and how it aligns with your policy coverage. Evidence from healthcare professionals can significantly strengthen your case. As specialists often say, "A letter from a doctor explaining medical necessity can greatly enhance an internal request."
- Policy Documents: Include your insurance policy documents that outline coverage for the denied service. Highlight the relevant sections that support your argument. Understanding your policy is essential for navigating the review process. Remember, insurers often send an insurance denial letter on the first review, hoping many policyholders will give up. Persistence is key!
- Additional Evidence: If you have it, gather extra evidence like test results, treatment plans, or letters from specialists. This additional documentation can further substantiate your case. For instance, Elena R. successfully appealed her $9,800 ER bill, saving $8,600 after demonstrating the necessity of her treatment.
Organize this information clearly and coherently. When you submit your request, reference each piece of evidence and explain how it supports your argument against the denial. This structured approach not only strengthens your case but also shows the insurer that you’re serious about receiving the benefits you deserve.
Engage Legal Support When Necessary
If you’re feeling overwhelmed by the request process or if your initial request has resulted in an insurance denial letter, it’s completely understandable. Seeking legal support can be a crucial step forward. Here’s how to approach this:
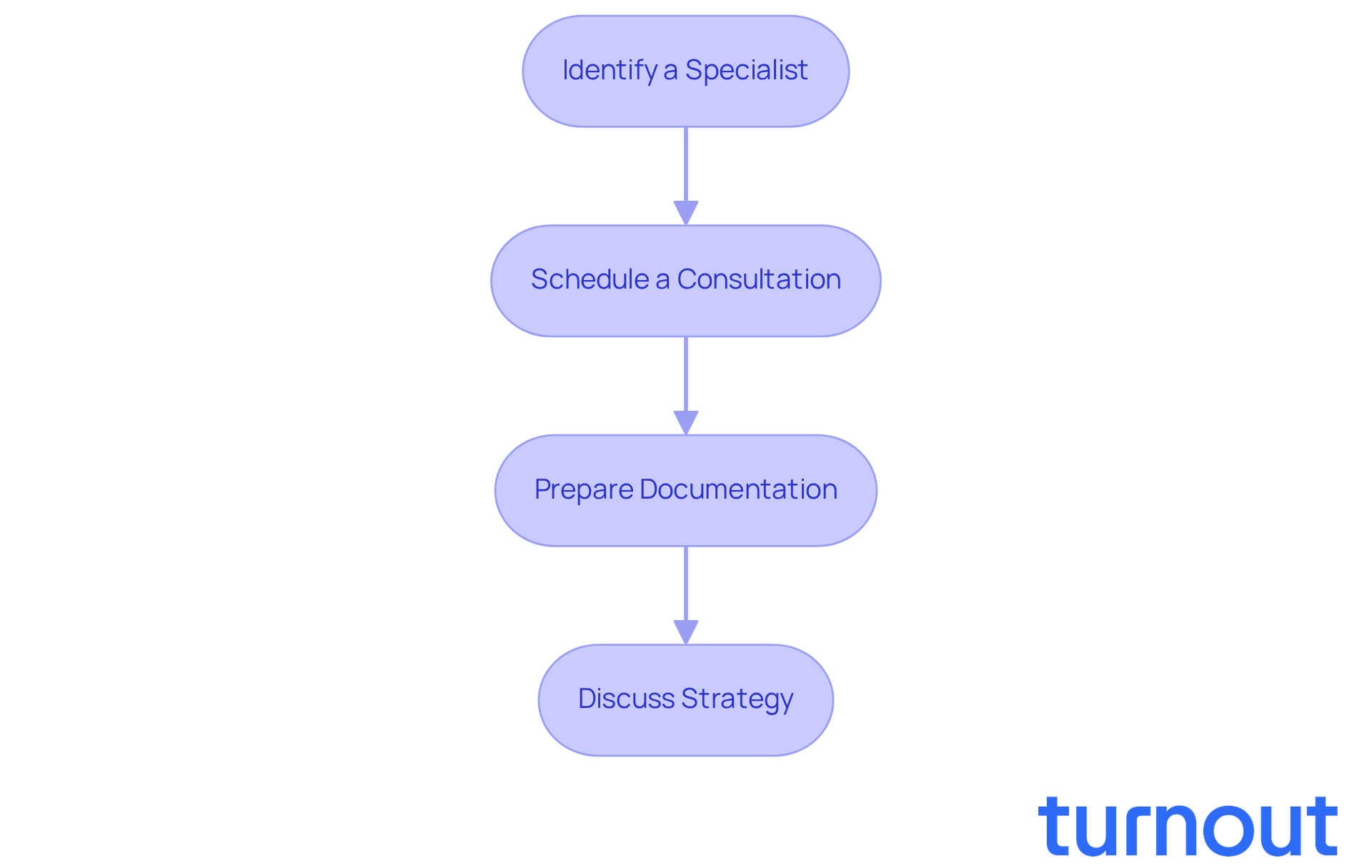
- Identify a Specialist: Look for attorneys or advocates who specialize in insurance claims or health law. Their expertise is vital for navigating the complexities of your case.
- Consultation: Schedule a consultation to discuss your situation. Many attorneys offer free initial consultations, allowing you to assess their approach and expertise without any financial commitment.
- Prepare Documentation: Gather all relevant documents, including the insurance denial letter, your request for reconsideration, and any supporting evidence. This preparation helps your attorney quickly grasp your circumstances and formulate a strategy.
- Discuss Strategy: Collaborate with your legal support to develop a customized approach for your case. They can clarify your rights and outline the best course of action moving forward.
Obtaining legal assistance not only enhances your understanding of the review process but also significantly boosts your chances of a favorable outcome. Did you know that over 50% of requests for coverage or reimbursement refusals in the medical sector lead to positive results, especially when legal knowledge is utilized? Legitimate claims or those rejected in bad faith often have favorable outcomes upon reconsideration. This makes it essential to seek advice from a lawyer if your claim is denied without adequate investigation. Remember, having a lawyer by your side can provide the reassurance and understanding needed to successfully contest a refusal. You are not alone in this journey.
Enhance Your Appeal with Strategic Documentation
Enhancing your attractiveness in the appeal process starts with comprehensive and well-organized documentation. We understand that this can feel overwhelming, but following these guidelines can make a significant difference:
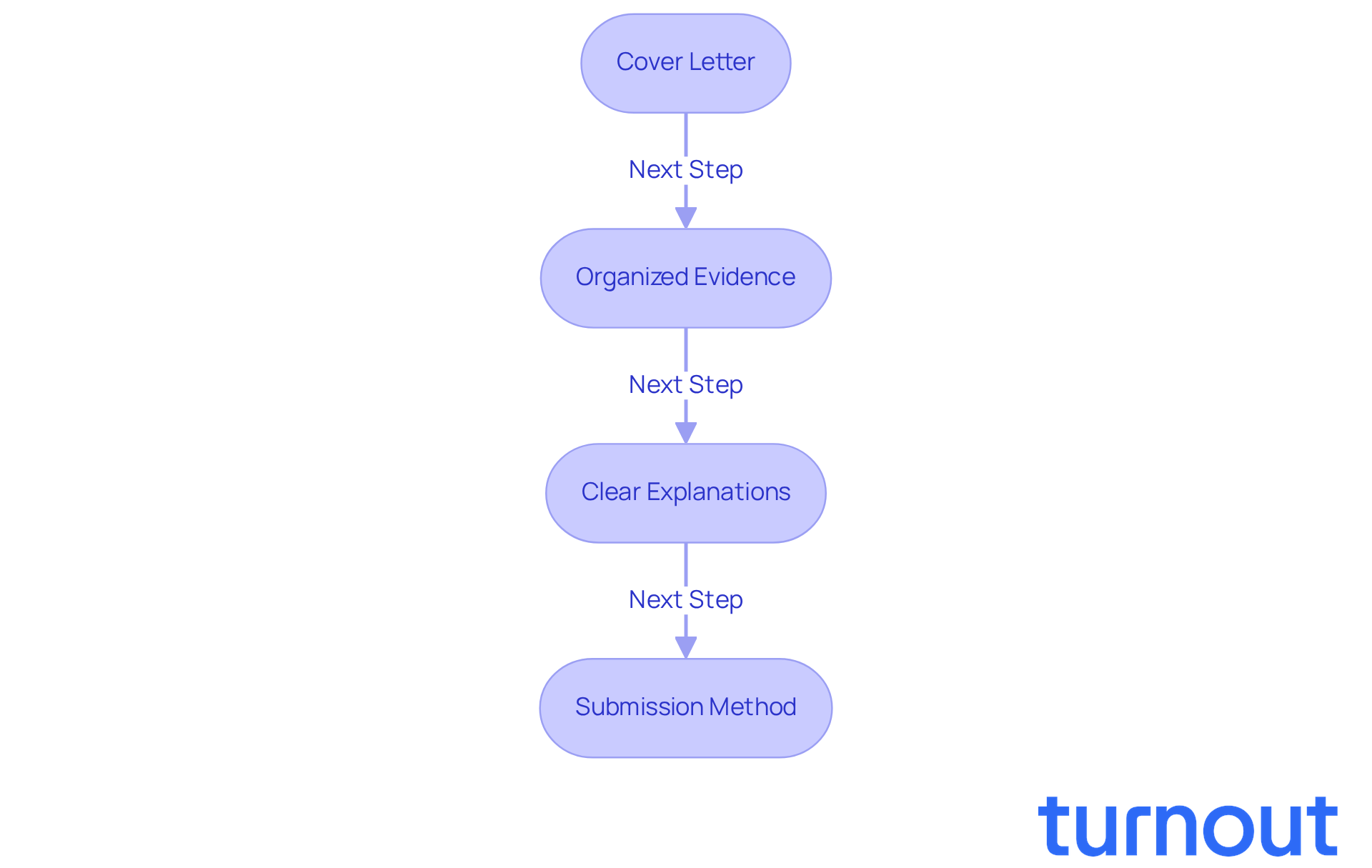
- Cover Letter: Begin with a clear cover letter. Outline your intent to appeal, summarize the reasons for the denial, and list the documents included in your appeal package. This sets a positive tone right from the start.
- Organized Evidence: Arrange your evidence logically. Using tabs or labels can help the reviewer navigate through your documents easily, making their job simpler and your case stronger.
- Clear Explanations: For each piece of evidence, provide a brief explanation of its relevance to your case. This helps the reviewer understand why each document supports your request, making your appeal more compelling.
- Submission Method: When sending your request, consider using certified mail or another trackable method. This ensures it’s received, and keeping copies of everything you send is a smart move for your records.
By enhancing your appeal with strategic documentation, you not only increase the likelihood of a favorable outcome but also demonstrate your commitment to resolving the issue. Remember, you are not alone in this journey; we’re here to help you every step of the way.
Conclusion
Mastering the response to an insurance denial letter is crucial for navigating the often complex and frustrating landscape of insurance claims. We understand that facing a denial can feel overwhelming, but by following four key steps:
- Reviewing the denial letter
- Disputing with strong evidence
- Engaging legal support when necessary
- Enhancing your appeal with strategic documentation
you can significantly increase your chances of overturning that denial.
Throughout this article, we’ve emphasized strategies designed to empower you in your claims process. Understanding the specific reasons for denial, gathering comprehensive documentation, and knowing when to seek legal assistance are all vital components in crafting a successful appeal. Remember, the importance of presenting your evidence in an organized and clear manner cannot be overstated; it directly influences the outcome of the reconsideration process.
Ultimately, taking proactive steps in response to an insurance denial not only enhances the likelihood of a favorable resolution but also instills confidence in you as you face these challenges. By equipping yourself with the right knowledge and resources, navigating the appeals process becomes less daunting. Embrace this opportunity to advocate for your rights-you are not alone in this journey, and we’re here to help ensure you receive the benefits you deserve.
Frequently Asked Questions
What should I do first when I receive an insurance denial letter?
Begin by carefully reviewing the denial letter to understand the specific reasons for the claim denial, which may include issues like lack of medical necessity, policy exclusions, or incomplete documentation.
What are common reasons for insurance claim denials?
Common reasons for denials include lack of medical necessity, policy exclusions, and incomplete documentation. For example, Cigna HealthCare of North Carolina noted that 30% of rejection reasons were due to medical necessity.
Why is it important to understand the policy language in the denial letter?
Understanding the policy language is essential because it helps you identify the insurer's justification for the denial and can assist you in crafting a persuasive request for reconsideration.
Are there deadlines I need to be aware of when submitting a request for reconsideration?
Yes, most insurers require requests for reconsideration to be submitted within a specific timeframe, typically ranging from 30 to 180 days depending on the plan. Missing these deadlines is a common reason for claim denials.
How can I ensure I have the correct contact information for my appeal?
Check the denial letter for the contact details of the department managing requests. This information is necessary for your next steps in the appeal process.
What can I do to improve my chances of a successful appeal?
By understanding the key components of the denial letter and addressing the insurer's concerns directly, you can effectively prepare for your request and increase your chances of a successful outcome.
What is an expedited appeal, and how quickly can it be reviewed?
An expedited appeal is a request for a faster review process for urgent situations, which can be reviewed in as little as 72 hours.




