Introduction
Navigating the labyrinth of insurance claims can often feel like an uphill battle. We understand that receiving a denial letter can leave you feeling frustrated and powerless. It's important to know that you're not alone in this journey. In fact, nearly 19% of denials stem from issues related to medical necessity alone.
This article offers a step-by-step guide on how to effectively respond to an insurance coverage denial. Our goal is to empower you to take control of your situation and potentially overturn that decision. But what happens when the initial rejection feels final? How can you craft a compelling appeal that not only addresses the insurer's concerns but also stands a chance against the daunting statistics of denial?
We’re here to help you navigate this process with confidence.
Identify the Reasons for Denial
Start by carefully reviewing the insurance coverage denial letter that you received from your provider. This insurance coverage denial letter should clearly outline the specific reasons for the denial, which may include lack of medical necessity, incomplete documentation, or policy exclusions. We understand that this can be frustrating, but paying close attention to any codes or terminology used can shed light on the insurer's decision-making process.
Did you know that a significant percentage of insurance claims - approximately 19% - are denied due to issues related to medical necessity? This highlights the importance of understanding these criteria. As Amanda Ledwich, a patient advocate, notes, "A lot of beneficiaries also don't know they can appeal. A denial will come in, and they're told 'no, sorry, that's it' when in fact they have that right."
If any reasons are unclear, please don’t hesitate to reach out to the insurance company for clarification. Remember, this understanding is crucial for crafting a compelling appeal that directly addresses the insurer's concerns. You're not alone in this journey, and we're here to help increase your chances of a successful outcome.
Document Key Details and Deadlines
Creating a dedicated folder for all documents related to your claim and rejection can make a world of difference. We understand that dealing with insurance can be overwhelming. This folder should include:
- The rejection document
- Your original claim
- Any communication with the insurance company
- Relevant medical records
It's crucial to note the deadlines for submitting a request, which are often specified in the insurance coverage denial letter. Mark these important dates on your calendar to ensure you submit your request on time. Additionally, keeping a log of any phone calls made regarding your claim - like dates, times, and the names of representatives you spoke to - can be incredibly helpful. This documentation will support your request, as studies show that organized submissions can increase success rates by up to 60%, according to healthcare advocates.
Remember, you typically have 180 days to submit your request after receiving the rejection notice. This timeframe is common across various health plans, so staying organized and proactive is essential. For instance, Elena R. successfully challenged her rejection for an emergency room bill by meticulously documenting her symptoms and interactions with her insurer, resulting in significant savings. You're not alone in this journey, and with the right approach, you can navigate this process successfully.
Craft a Formal Appeal Letter
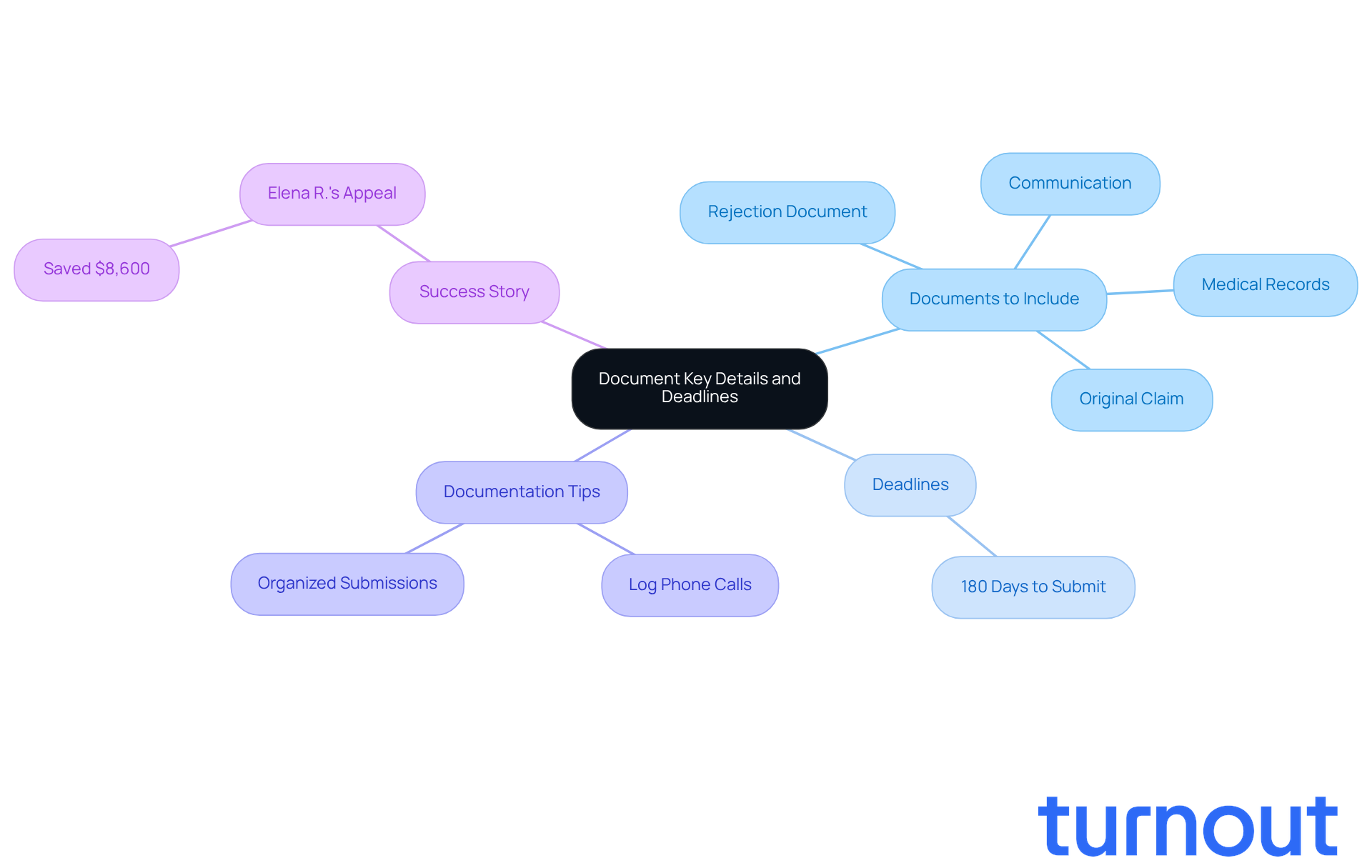
When you're faced with an insurance claim rejection, it can feel overwhelming. We understand that this is a challenging situation, and we're here to help you navigate it. Start your appeal by placing your contact details, the date, and the insurance company's address at the top of your letter. Clearly state that you are contesting the refusal of your claim by referencing the specific insurance coverage denial letter, including its date and any relevant claim numbers.
In the body of your letter, briefly summarize why you believe the rejection was incorrect. Support your case with proof from your medical records and policy documents. Include details about the denial and explain why you think an error has been made. Maintaining a professional tone is crucial, so ensure your points are clear and well-supported. Conclude by requesting a thorough review of your claim and include your contact information for any necessary follow-up. To ensure your correspondence is received, consider sending it via certified mail.
Effective communication is key. For instance, Jennifer's appeal included research studies and a note from her oncologist, which ultimately led to the reversal of her rejection. Similarly, Michael's request for a specialized wheelchair was successful thanks to comprehensive assessments from specialists.
Here are some key components of an effective appeal letter:
- A clear statement of the appeal
- Reference to the denial letter and claim details
- Evidence supporting your case, such as medical records and policy provisions
- A professional and respectful tone
- A request for a review of the claim
Insurance professionals agree that a well-structured appeal letter can significantly increase your chances of a successful outcome. Some studies even indicate that thorough documentation and clear communication can enhance approval rates by up to 60%. If your internal request is denied, remember that you have the right to ask for an independent review organization (IRO) to assess your case. By following these guidelines, you can effectively advocate for your rights and improve your chances of overturning a denial.
Don't forget to keep all correspondences, notes, and records organized in one place for quick reference during the review process. Lastly, inquire about the availability of a Consumer Assistance Program in your state, as this can provide additional support in navigating the review process. You're not alone in this journey, and with the right approach, you can find the assistance you need.
Follow Up on Your Appeal Submission
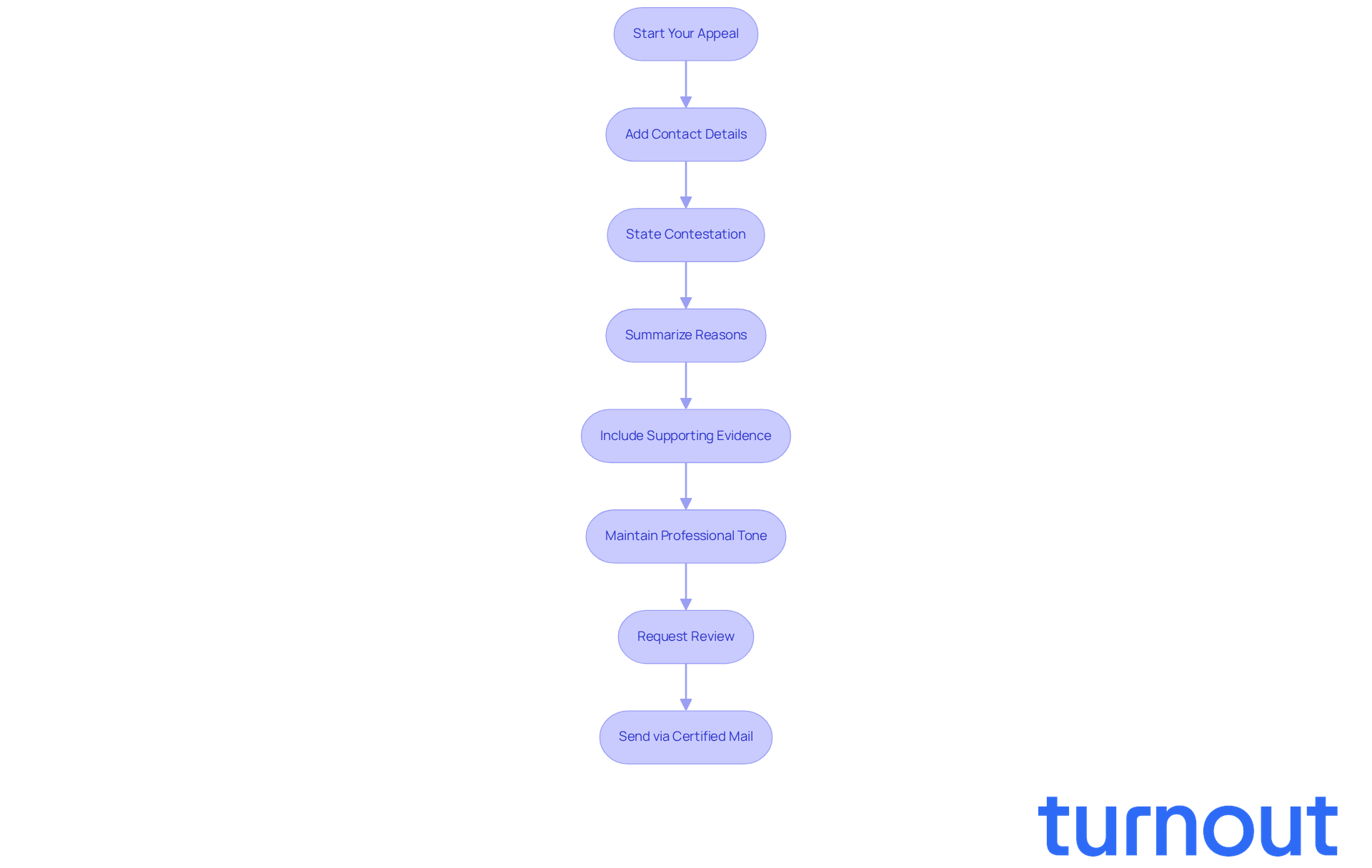
After sending your request, it’s important to check back with the provider. We understand that this process can be stressful. Call the customer service number provided in the insurance coverage denial letter or on your insurance card. Request confirmation that your request has been received and ask about the anticipated timeline for a decision, which usually spans from 30 to 180 days.
Keep a record of this conversation, including the date, time, and the name of the representative you spoke with. If you don’t receive a response within the specified timeframe, don’t hesitate to reach out again. Remember, persistence is key. Research shows that submitting a request for an insurance coverage denial letter puts you ahead of 99% of consumers who accept refusals without hesitation. In fact, 44% of internal requests succeed in overturning denials, highlighting the potential success of your efforts.
Successful follow-up strategies include:
- Sending a follow-up email summarizing your previous conversation and reiterating your request for a timely response.
- Considering using AI-powered appeal letter generators to help craft effective appeals.
Staying proactive can significantly increase your chances of a favorable outcome. You are not alone in this journey; we’re here to help.
Conclusion
Navigating an insurance coverage denial can feel overwhelming, and we understand how frustrating this process can be. However, knowing how to respond effectively is essential for securing the coverage you deserve. By following these steps, you can significantly improve your chances of overturning a denial.
- First, it’s crucial to identify the reasons for the denial.
- Take the time to document all related details meticulously.
- Next, craft a compelling appeal letter that clearly outlines your case.
- Don’t forget the importance of maintaining proactive follow-up communication with your insurance provider.
Each of these steps empowers you to advocate for your rights confidently. Remember, organized submissions can improve success rates by up to 60%! This guidance is not just practical; it’s essential.
The journey through insurance claim denials may be daunting, but persistence truly pays off. By taking informed action and utilizing available resources, you can effectively challenge denials and advocate for your healthcare needs. Embrace the power of knowledge, and remember, you are not alone in this journey. We’re here to help you ensure that your voice is heard in the insurance process.
Frequently Asked Questions
What should I do first when I receive an insurance coverage denial letter?
Start by carefully reviewing the denial letter, which should outline the specific reasons for the denial, such as lack of medical necessity, incomplete documentation, or policy exclusions.
Why are insurance claims often denied?
Approximately 19% of insurance claims are denied due to issues related to medical necessity, making it important to understand these criteria.
Can I appeal an insurance coverage denial?
Yes, you have the right to appeal an insurance coverage denial. Many beneficiaries are unaware of this right, so it’s important to take action if you believe the denial was unjust.
What should I do if I don’t understand the reasons for my denial?
If any reasons for the denial are unclear, reach out to the insurance company for clarification. Understanding the reasons is crucial for crafting a compelling appeal.
How can understanding the denial reasons help me?
Understanding the reasons for the denial can help you craft a compelling appeal that directly addresses the insurer's concerns, increasing your chances of a successful outcome.




