Introduction
Navigating the complexities of insurance claims can often feel like an uphill battle. We understand that receiving a denied claim letter can be disheartening. However, understanding the intricacies of the denial process is crucial. It presents an opportunity for you to reclaim what you are rightfully owed.
So, how can you effectively respond to a denial and increase your chances of a successful appeal? This guide breaks down the essential steps to take when faced with a denied claim. We’re here to empower you to tackle this situation with confidence and clarity. Remember, you are not alone in this journey.
Review the Denial Letter Thoroughly
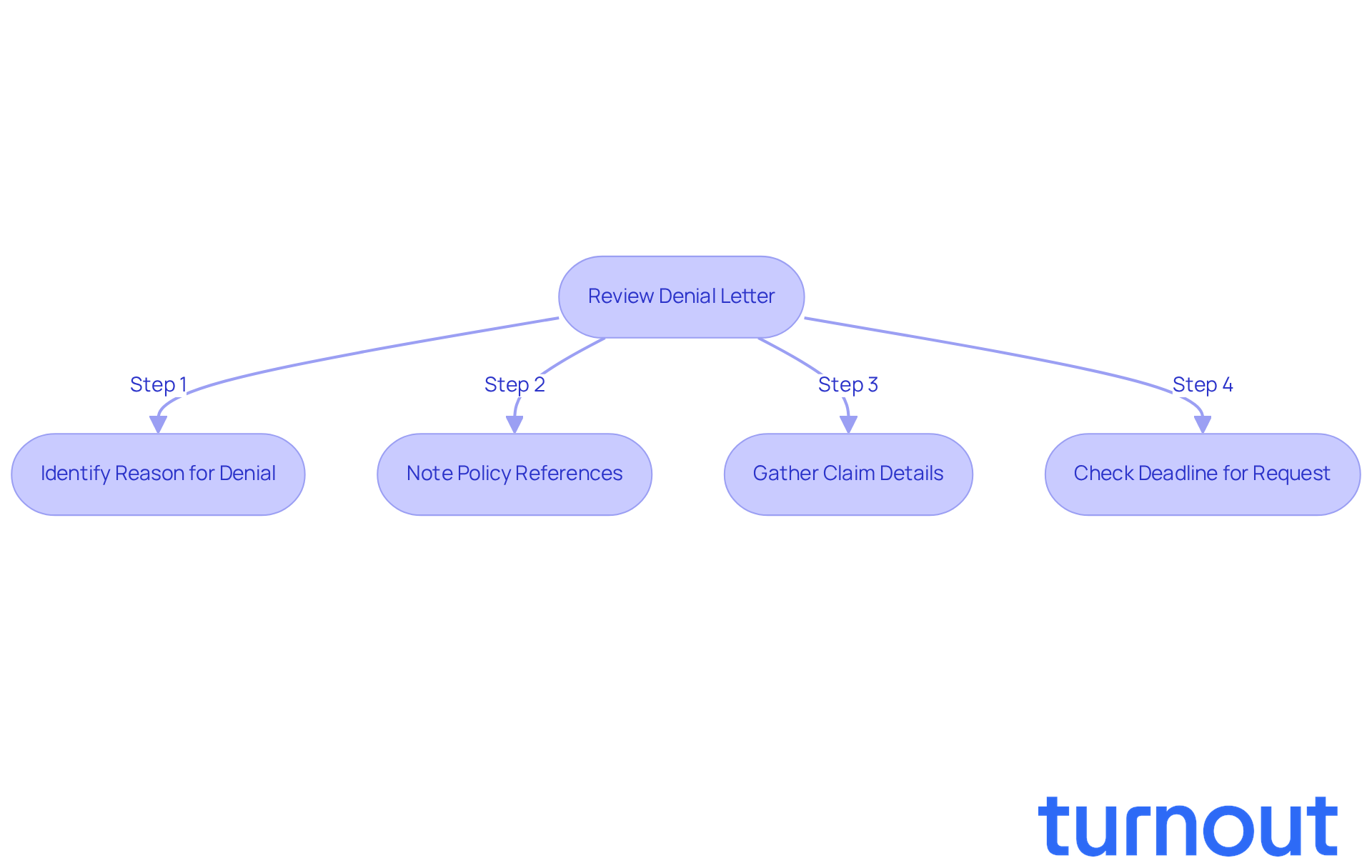
Begin by thoroughly reviewing the denied claim letter from top to bottom. We understand that this can be a frustrating process, so let’s break it down together. Pay close attention to these key components:
-
Reason for Denial: Identify the specific reasons cited by the insurer. Common issues include lack of medical necessity, incomplete documentation, or policy exclusions. Understanding these reasons is essential for crafting a persuasive denied claim letter.
-
Policy References: Take note of any specific policy clauses referenced by the insurance provider that justify the denial. This information is crucial for your request, as it enables you to directly address the insurer's statements in the denied claim letter.
-
Claim Details: Ensure you have all relevant claim information, including the claim number, date of service, and any other identifiers. This data will be necessary when composing your request letter.
-
Deadline for Request: Check the timeline provided for submitting your request. Most insurers allow a specific timeframe, often up to 180 days, to challenge a refusal. Adhering to this timeline is critical to ensure your appeal regarding the denied claim letter is considered.
It’s common to feel overwhelmed by this process, but statistics suggest that around half of rejected requests are successfully appealed, especially when backed by comprehensive documentation and a clear understanding of the denial reasons. Keeping detailed records of all communications with insurance representatives can significantly bolster your case. If you find the process daunting, remember that consulting a lawyer experienced in insurance matters can offer valuable advice and enhance your chances of a successful outcome. We're here to help you navigate this journey.
Gather Supporting Evidence for Your Appeal
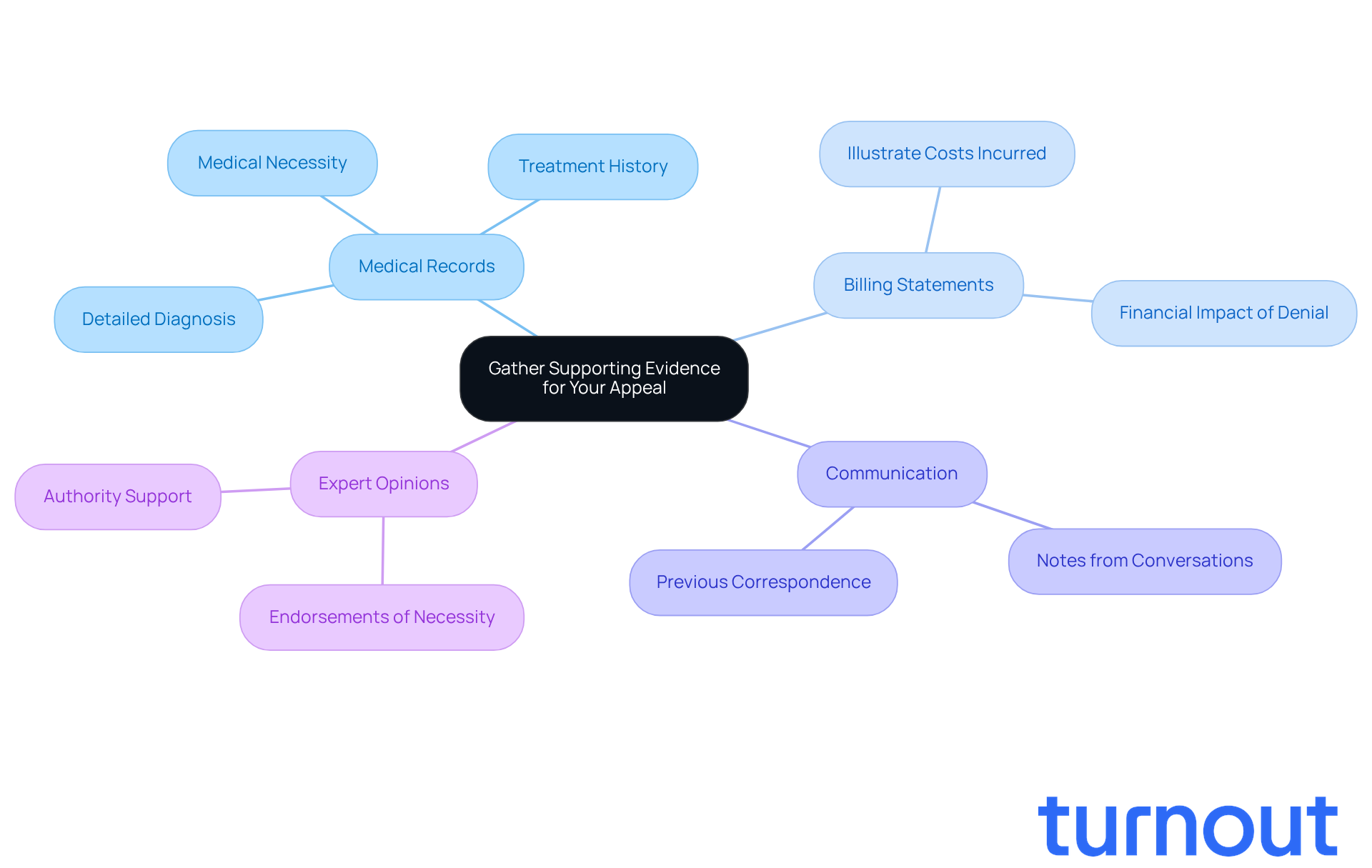
To enhance your appeal, it’s essential to gather all relevant documents that support your claim. This includes:
- Medical Records: Secure detailed medical records from your healthcare provider that clearly outline your diagnosis, treatment history, and the medical necessity of the services rendered. A well-documented medical history can significantly strengthen your case, as insurers often rely on this information to assess the legitimacy of requests.
- Billing Statements: Include any bills related to the denied request to illustrate the costs incurred. These statements provide concrete evidence of the financial impact of the denial and clarify the necessity of the services.
- Communication: Collect any previous communication with the insurance provider regarding the request, including notes from phone conversations or emails. Keeping a record of these communications can reveal discrepancies in the insurer's handling of your claim and support your request.
- Expert Opinions: If applicable, consider obtaining a statement from a medical expert that endorses the necessity of the treatment or service. Such endorsements can lend authoritative support to your request, enhancing its credibility.
Organizing these documents clearly is vital; a well-structured submission can greatly influence the review process. Statistics show that successful insurance requests often include an average of 10 to 15 documents, underscoring the importance of careful preparation. Many insurance requests for reconsideration fail because the patient did not address the specific concerns mentioned in the denied claim letter. It’s crucial to respond directly to the reasons provided in the denied claim letter. By addressing these specific reasons and providing comprehensive evidence, you increase your chances of a favorable outcome. Remember, urgent requests can be processed in as little as 4 days when health is at risk, so timely submissions are essential. As Scott Friedson wisely notes, "most denials are not the final word; they are an opening move in a negotiation.
Draft a Persuasive Appeal Letter
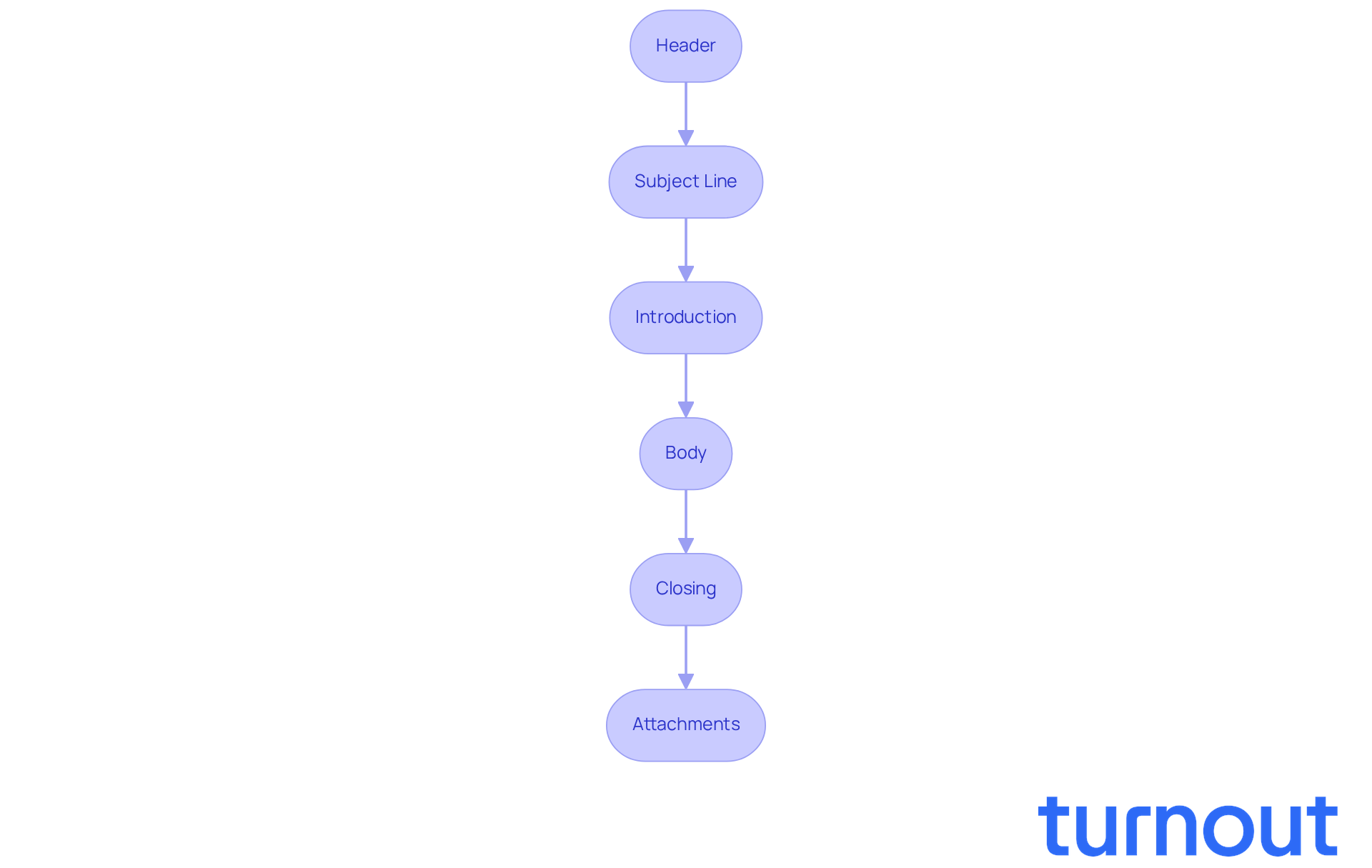
When writing your appeal letter, it’s important to follow a thoughtful structure that reflects your concerns and hopes:
- Header: Start with your name, address, and contact information at the top. Then, include the date and the insurer's address.
- Subject Line: Clearly state the purpose of your letter, such as 'Appeal of Denied Claim Letter [Claim Number].'
- Introduction: Briefly introduce yourself and express the purpose of your letter. You’re reaching out for support, and that’s perfectly okay.
- Body:
- State the Facts: Summarize your claim and the reason it was denied. It’s important to be clear and factual here.
- Present Your Argument: Use the evidence you’ve gathered to counter the reasons for rejection. Stick to the facts, and avoid emotional language, even though it’s a tough situation.
- Request Action: Clearly state what you would like the insurance provider to do, like overturning the denial. Be direct but gentle in your request.
- Closing: Thank the insurer for their time and express your hope for a favorable resolution. A little gratitude goes a long way.
- Attachments: List the documents you’re including with the letter to support your case.
Remember, your letter should be concise, professional, and free of errors. We understand that this process can be overwhelming, but you’re not alone in this journey. We’re here to help.
Submit Your Appeal Before the Deadline
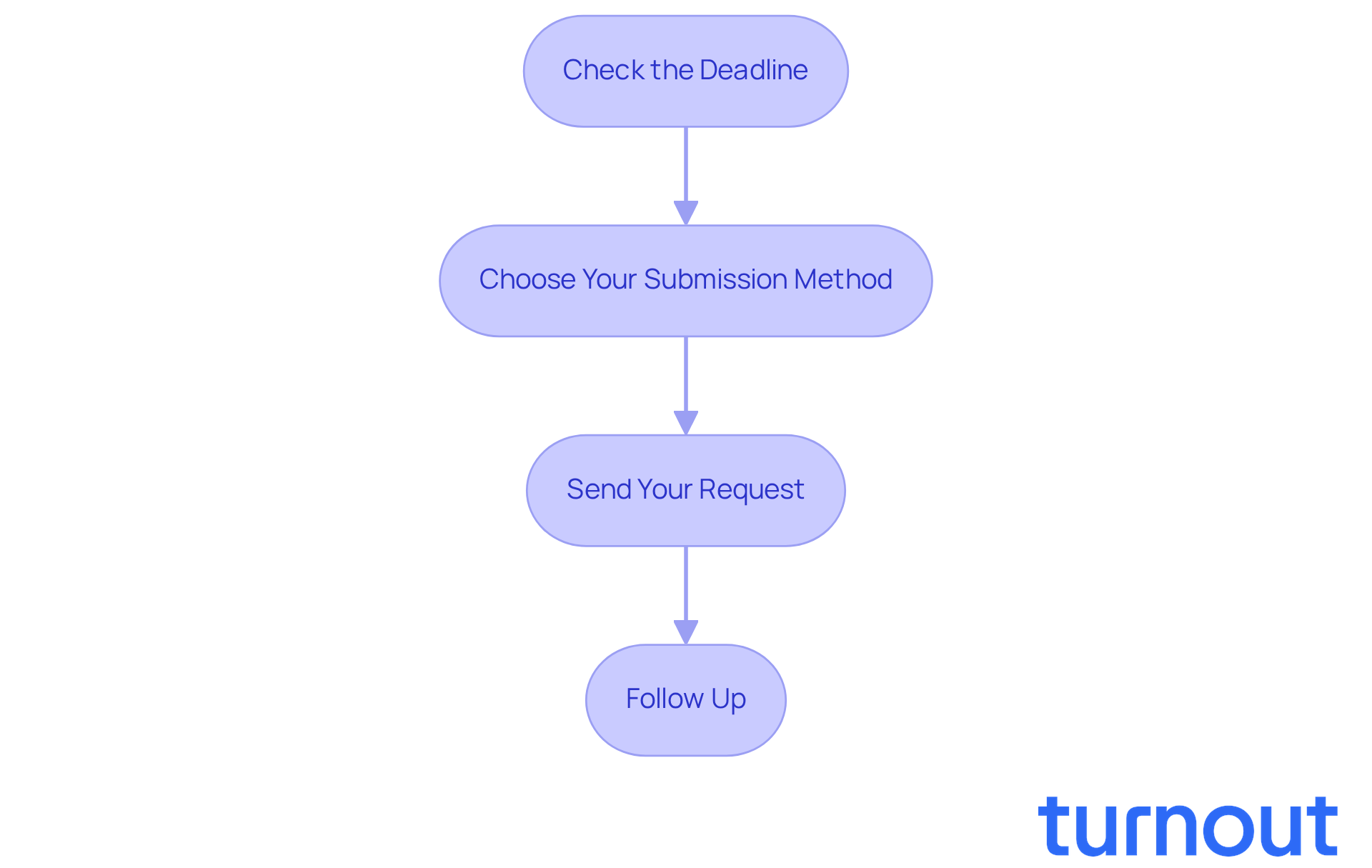
Once your request letter and supporting documents are ready, it’s important to submit your case effectively. We understand that this process can feel overwhelming, but following these steps can help you navigate it with confidence:
- Check the Deadline: Take a moment to verify the submission deadline mentioned in the denial letter. Mark it on your calendar. Insurance companies often have strict timelines for handling disputes, including a requirement to make decisions on internal challenges for treatments already received within 60 days. Being aware of these dates is essential for timely submissions.
- Choose Your Submission Method: Most providers accept submissions via mail, fax, or online portals. Select the method that best fits your situation, ensuring it allows for tracking your submission. This is vital, as timely follow-up can significantly impact the outcome.
- Send Your Request: If you decide to mail your request, consider using certified mail with a return receipt to confirm delivery. For fax or online submissions, keep a copy of the confirmation. This documentation can be crucial if any disputes arise regarding the denied claim letter.
- Follow Up: After submitting your request, promptly follow up with the insurer to confirm receipt and ask about the expected timeline for a decision. Insurers must address internal requests for treatments already received within 60 days, and for urgent care claims, within 72 hours. Keeping detailed notes of all conversations with insurance representatives, including names, dates, and times, is also recommended to ensure effective communication.
By following these steps and ensuring your request is submitted on time, you enhance your chances of a favorable outcome. Remember, persistence is key; many successful requests arise from diligent follow-up and clear communication with the insurer. For example, a client at a dialysis facility faced underpayments but achieved success after persistent follow-up and appeals. This illustrates the importance of not giving up. We're here to help you through this journey.
Conclusion
Navigating the complexities of a denied insurance claim can feel overwhelming. We understand that this process can be daunting, but knowing how to approach it is essential for a successful appeal. Responding effectively to a denial letter requires a systematic approach:
- Review the denial thoroughly
- Gather supporting evidence
- Draft a persuasive appeal letter
- Submit it before the deadline
By following these steps, you can significantly improve your chances of overturning the denial.
Key insights from this guide highlight the importance of addressing the reasons for denial comprehensively. Utilize detailed documentation and maintain clear communication with your insurance provider. Each step, from understanding the denial letter to crafting a well-structured appeal, plays a vital role in strengthening your case. Did you know that many denied claims can be successfully appealed? With diligence and a strategic mindset, you can turn the situation around.
Ultimately, persistence and preparation are crucial in the appeal process. Taking the time to gather the necessary evidence and submit your appeal on time not only enhances your likelihood of success but also empowers you to advocate for your rights. Remember, you are not alone in this journey. By approaching the situation with confidence and clarity, you can navigate the insurance landscape more effectively and ensure that your claims receive the consideration they deserve.
Frequently Asked Questions
What should I do first when I receive a denial letter for my insurance claim?
Begin by thoroughly reviewing the denied claim letter from top to bottom, paying close attention to the key components outlined in the letter.
What are the common reasons for an insurance claim denial?
Common reasons include lack of medical necessity, incomplete documentation, or policy exclusions.
Why is it important to note policy references in the denial letter?
Noting specific policy clauses referenced by the insurer is crucial as it helps you directly address the insurer's statements in your request for appeal.
What claim information should I gather before composing my request letter?
Ensure you have all relevant claim information, including the claim number, date of service, and any other identifiers.
Is there a deadline for submitting a request to challenge a claim denial?
Yes, most insurers allow a specific timeframe, often up to 180 days, to challenge a refusal, so it's critical to adhere to this timeline.
What are the chances of successfully appealing a denied claim?
Statistics suggest that around half of rejected requests are successfully appealed, especially when backed by comprehensive documentation and a clear understanding of the denial reasons.
How can I strengthen my appeal for a denied claim?
Keeping detailed records of all communications with insurance representatives can significantly bolster your case.
What should I do if I find the appeal process overwhelming?
If the process feels daunting, consider consulting a lawyer experienced in insurance matters for valuable advice and to enhance your chances of a successful outcome.




