Introduction
Understanding the relationship between sleep apnea and various secondary conditions is crucial for veterans looking to improve their health and secure necessary benefits. Many former military personnel face challenges like anxiety, PTSD, and obesity, all linked to sleep apnea. Recognizing these connections can open important pathways to better disability ratings and support.
We understand that navigating these issues can feel overwhelming. It’s common to wonder how these conditions intertwine and what steps you can take to ensure your claims reflect the full extent of your health challenges.
You are not alone in this journey. We're here to help you understand the importance of these connections and how they can impact your well-being. By acknowledging your struggles and seeking the right support, you can take meaningful steps toward improving your health.
Anxiety as a Secondary Condition to Sleep Apnea
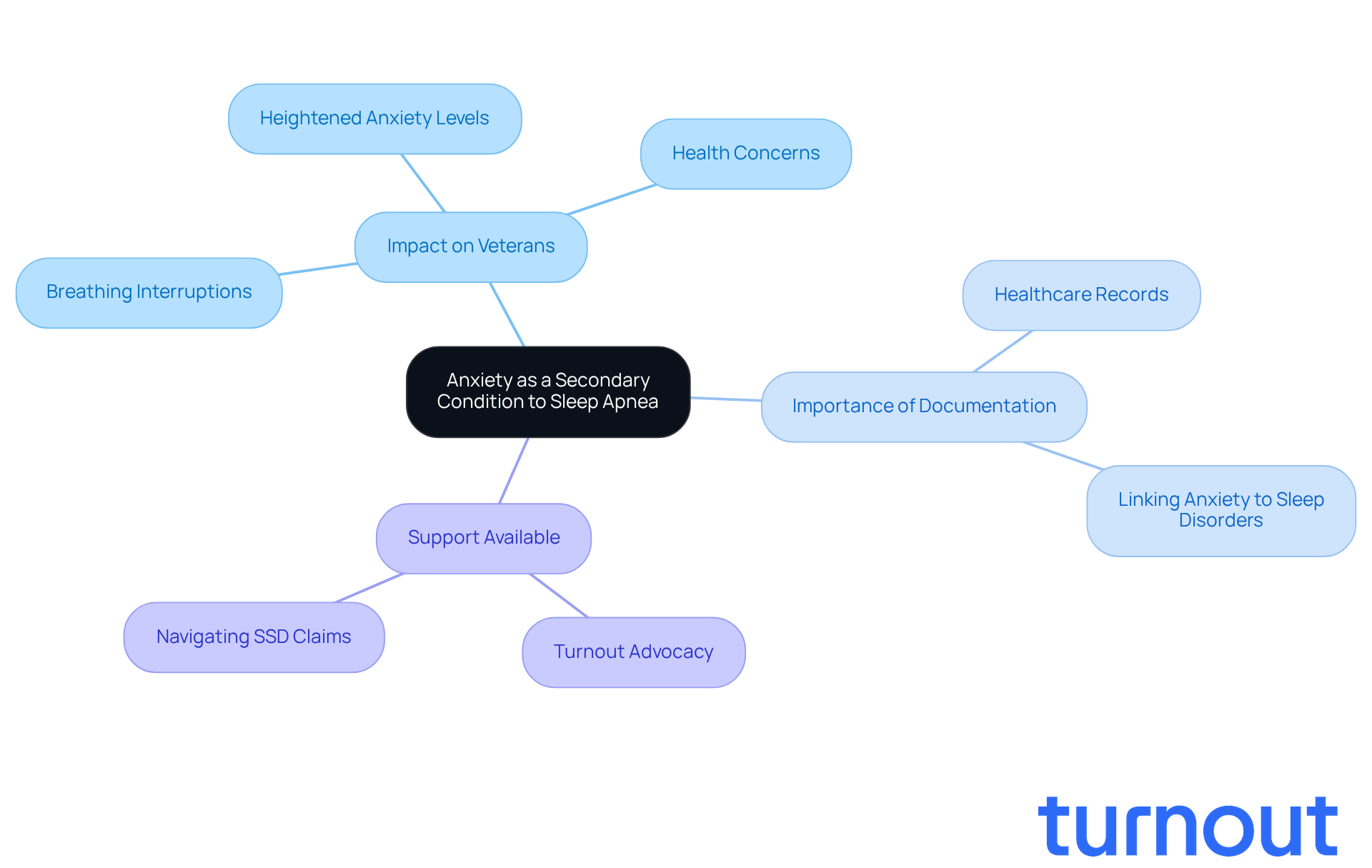
Anxiety is a common issue, especially those who experience anxiety. These issues often stem from the stress and fear linked to sleep apnea. We understand that this can lead to depression, which may worsen overall health.
For many ex-servicemen, anxiety often accompanies these challenges. This highlights how interconnected these issues can be. Recognizing these conditions is crucial for treatment, as it can potentially improve outcomes.
To strengthen their claims, veterans should gather evidence that clearly links their conditions. This documentation can significantly support the benefits they deserve.
At Turnout, we’re here to help veterans. Our trained staff are dedicated to assisting veterans with their claims, ensuring they receive support. Remember, you are not alone in this journey.
Asthma Linked to Sleep Apnea
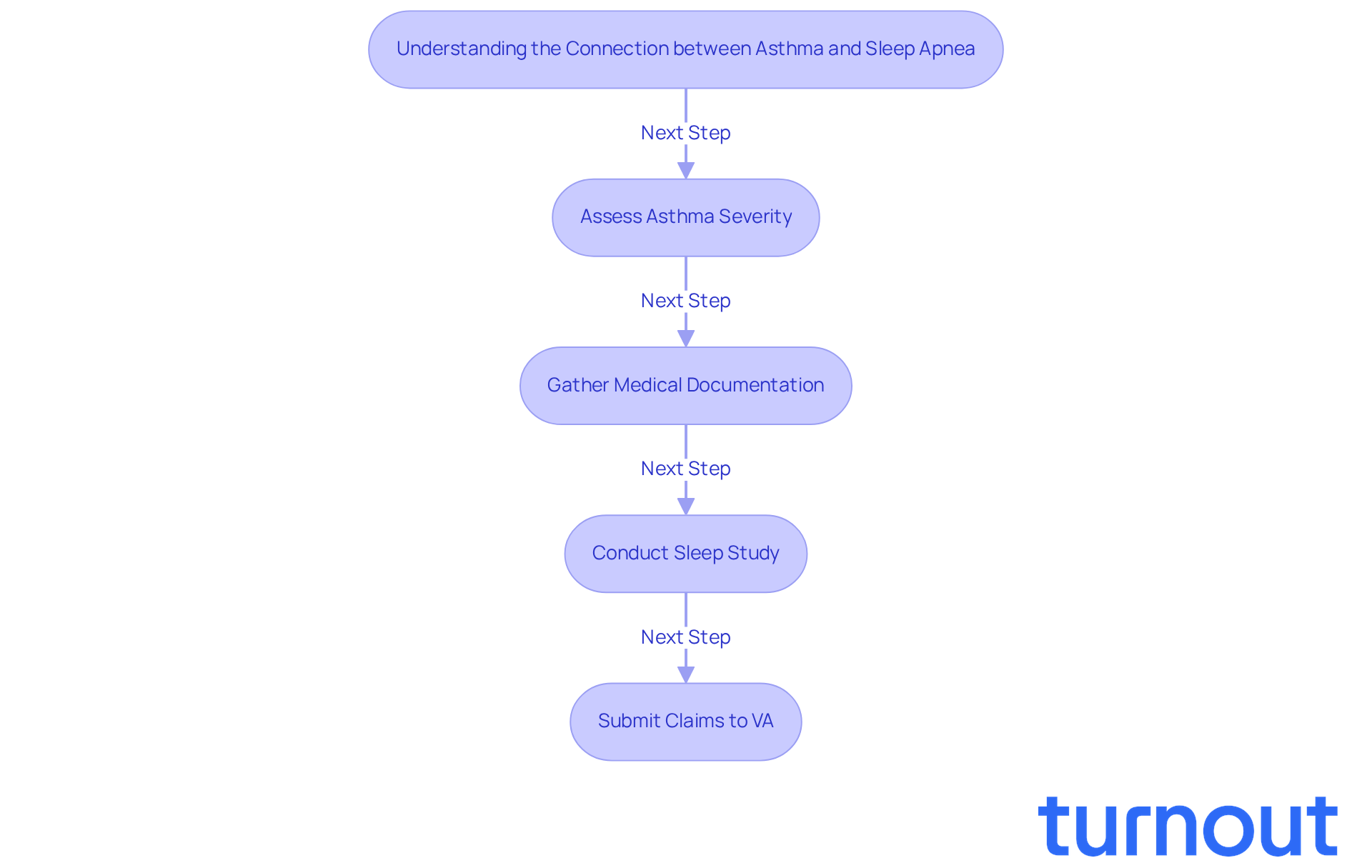
Asthma and sleep apnea often go hand in hand, and we understand how challenging this can be. These conditions can worsen symptoms, leading to complications. It’s concerning to know that individuals with asthma face nearly a 40% higher risk of developing sleep apnea compared to those without asthma.
This connection is particularly significant for veterans. The VA and recognizes the link by allowing for additional benefits requests. To address this, understanding their health conditions and its impact during rest is essential. This evidence is crucial for obtaining necessary treatments.
Moreover, a comprehensive approach for managing asthma is vital. This highlights the importance of coordinated care. As pulmonologists note, managing asthma in patients with sleep apnea requires diligence to optimize treatment outcomes.
Remember, you are not alone in this journey. We’re here to help you through the process and ensure you receive the support you need.
Post-Traumatic Stress Disorder as a Secondary Condition to Sleep Apnea
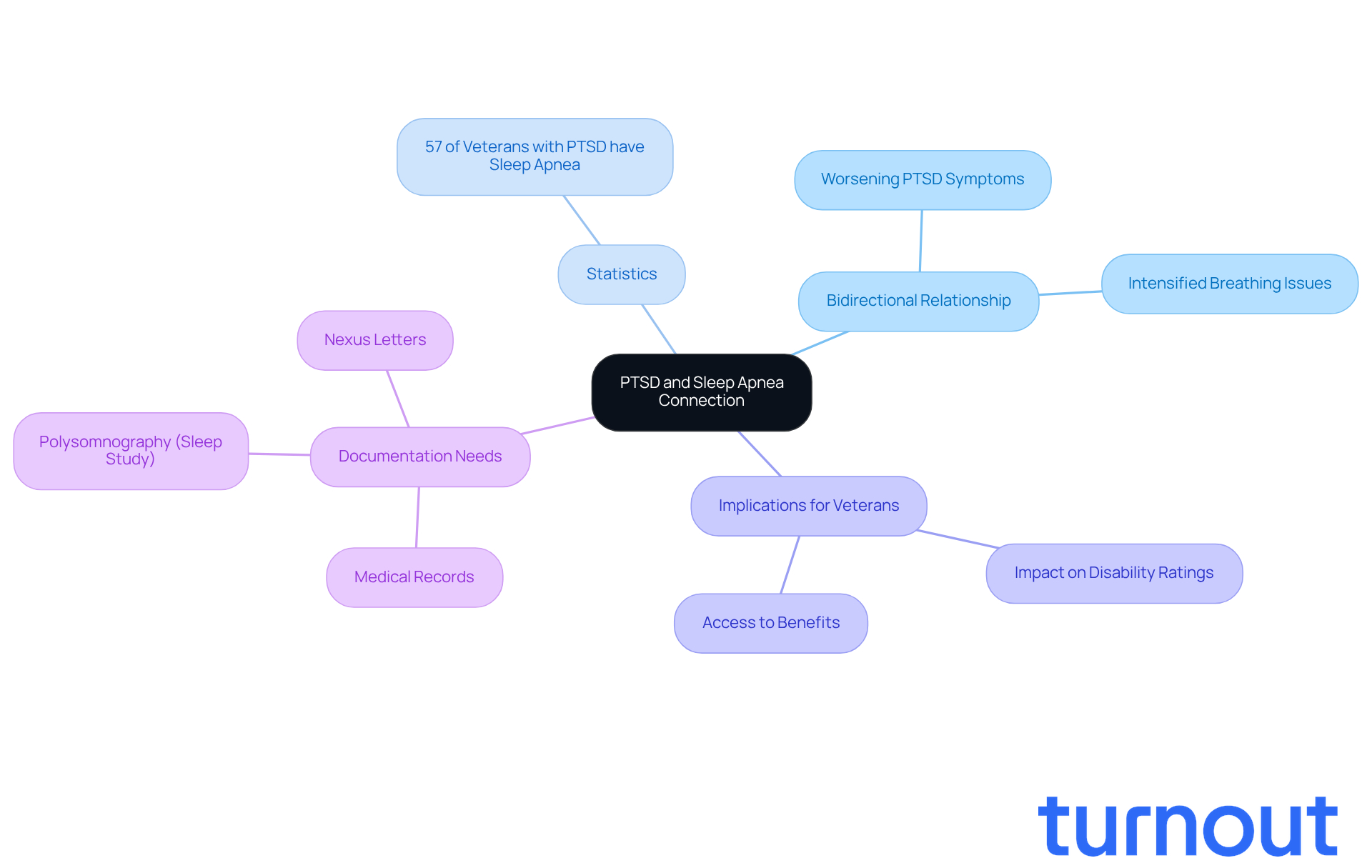
The connection between PTSD and sleep apnea is particularly significant for former military personnel. We understand that sleep disorders can deeply affect the mental health. Current research highlights that interrupted breathing can worsen PTSD symptoms, while the distress from PTSD can intensify breathing issues. This cycle can lead to increased daytime fatigue, irritability, and difficulty concentrating.
Did you know that veterans also have PTSD? This statistic underscores the commonality of this dual diagnosis. For many veterans, comprehensive documentation is crucial for their claims. Medical records, study results, and personal accounts can strengthen their case for compensation.
Furthermore, a thorough evaluation is essential to address their claims related to sleep apnea. By addressing their claims related to PTSD, veterans can better navigate the claims process. Remember, you are not alone in this journey; we’re here to help you.
Gastroesophageal Reflux Disease (GERD) Secondary to Sleep Apnea
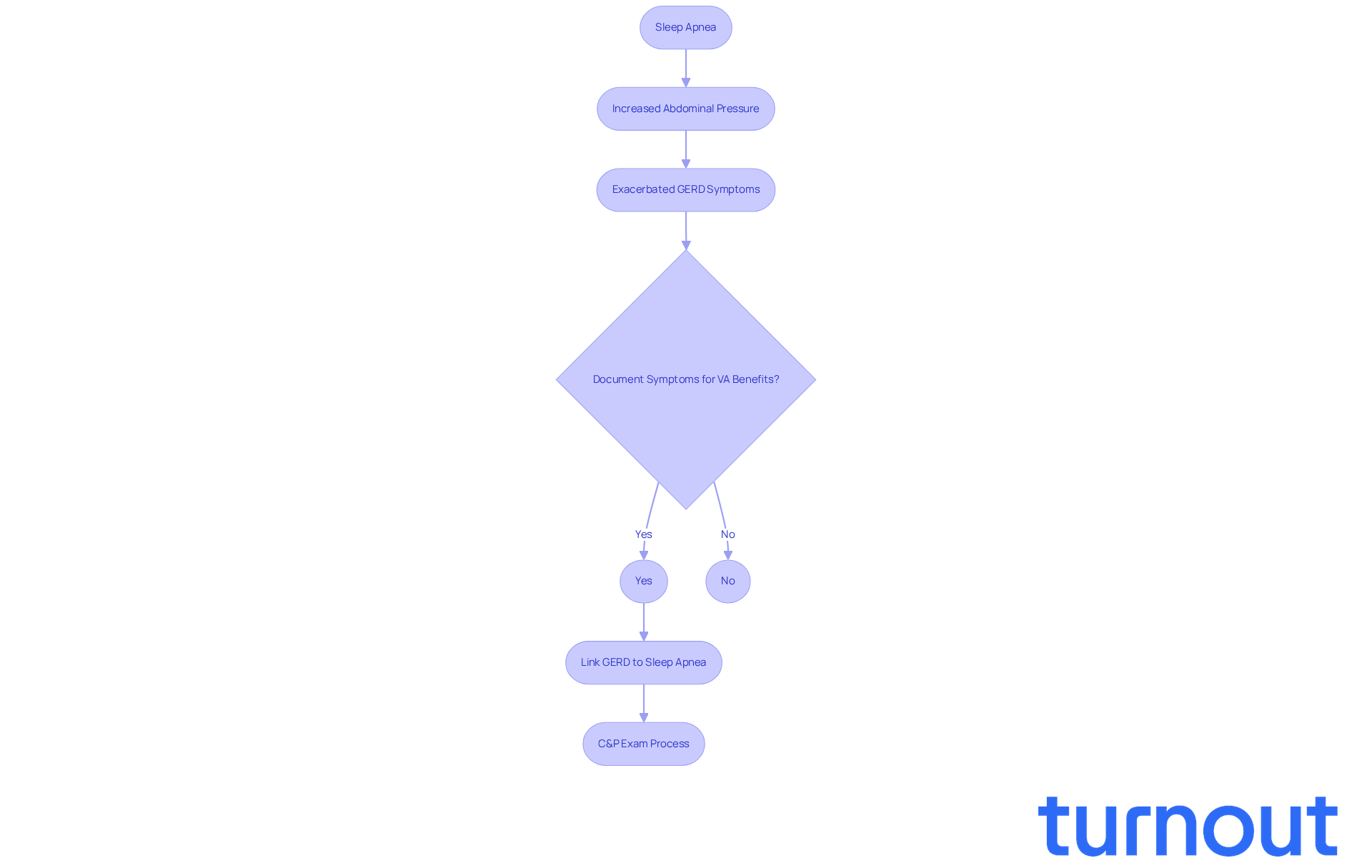
can be a challenging companion for many, especially for those who experience discomfort during rest. This often happens due to increased abdominal pressure during apneic episodes, which can intensify reflux symptoms. We understand that this can lead to complications. Research indicates that former service members with sleep apnea are more likely to develop GERD, as airway blockages can exacerbate the condition. For example, studies reveal that:
- 47 percent of patients with sleep apnea experience GERD, while
- it.
This can even further complicate their health.
When seeking treatment, it’s crucial for veterans to recognize and clearly link them as secondary conditions. This careful documentation can greatly strengthen their claims, as establishing a connection is vital for approval. Gastroenterologists emphasize the importance of recognizing this connection. They note that common symptoms, such as heartburn, regurgitation, and difficulty swallowing, should not be overlooked. As April Donahower wisely points out, 'If the individual has previously been diagnosed with sleep apnea, but has not undergone a formal evaluation, the VA will not consider that diagnosis as sufficient evidence for verifying eligibility for benefits.'
We encourage veterans to actively discuss these symptoms with their healthcare providers. This proactive approach ensures clarity and support throughout the claims process. Additionally, understanding the evaluation process is essential. This exam assesses the severity and cause of the veteran's condition and its implications. Remember, you are not alone in this journey, and we’re here to help.
Hypothyroidism as a Secondary Condition to Sleep Apnea
Hypothyroidism can significantly impact breathing interruptions during rest, often leading to changes in the upper airway that may worsen symptoms. We understand that this can be concerning. Recent research indicates that untreated hypothyroidism can lead to complications. For instance, a staggering 74% of hypothyroid patients were diagnosed with obstructive sleep apnea, highlighting how prevalent this condition is in this demographic. Moreover, studies showed an even higher prevalence of OSA at 85.3%, compared to 66.1% in those undergoing treatment. This suggests that effectively managing hypothyroidism is crucial for improving sleep apnea outcomes.
Patients with hypothyroidism, in particular, should prioritize sleep quality. Regular monitoring, particularly as symptoms can vary, is crucial for their overall health. It's common to feel overwhelmed by these challenges, especially as the average age of individuals with OSA tends to be higher among those with hypothyroidism. This underscores the need for comprehensive care.
Furthermore, the relationship between hypothyroidism and sleep apnea is still being explored. Evidence shows that lower free T4 levels and higher TSH levels are often found in individuals with OSA. This highlights the importance of recognizing secondary conditions to sleep apnea, particularly as they can minimize potential health complications. Remember, you are not alone in this journey, and seeking help can make a significant difference.
Tinnitus Linked to Sleep Apnea
Tinnitus is a challenge many face, especially those who have served in the military. We understand that this condition can be particularly distressing. Recent studies suggest that these interruptions, often linked to hypoxia, may worsen or even trigger tinnitus. Did you know that around 20% of people experience tinnitus at some point in their lives? This figure is especially significant for veterans dealing with sleep apnea, who might experience anywhere from one to 100 interruptions per hour while resting.
Chronic low oxygen levels can harm the delicate cochlear hair cells in the inner ear over time, potentially leading to tinnitus. Research shows that former service members with sleep apnea during rest are more likely to report tinnitus. This can greatly affect daily activities and overall quality of life. Moreover, nighttime sleep disturbances can cause vascular inflammation, which may hinder blood circulation to auditory structures, complicating the relationship between these conditions.
It's essential for veterans to document their symptoms and how they relate to sleep apnea when applying for benefits. This careful record-keeping can significantly strengthen a claim. If you have been diagnosed with both conditions, we encourage you to seek a medical evaluation to support your claim. This could help you secure the benefits you deserve.
When submitting your claim related to tinnitus, remember to include a detailed statement, medical records, and witness statements. These elements are crucial for a successful claim. You're not alone in this journey, and we're here to help you navigate the process.
Sinusitis as a Secondary Condition to Sleep Apnea
Sinusitis can lead to nasal congestion, making it hard to breathe comfortably, especially during rest. This connection is particularly significant for veterans. Untreated sinusitis can severely affect the quality of life, characterized by prolonged inflammation and swelling of the sinuses, can complicate nighttime breathing, increasing the likelihood of sleep disturbances.
Therefore, it’s crucial to ensure that your medical records accurately reflect any diagnosis and its link to respiratory issues, particularly the symptoms experienced during rest. This step can enhance your chances of receiving benefits. Did you know that around 22 million Americans suffer from sleep apnea? This makes it a common condition.
Establishing a clear connection between sinusitis and sleep apnea is essential. It may help you qualify for disability benefits, which can significantly improve your quality of life and access to healthcare services. To strengthen your claims, we encourage you to consult with professionals. They can assist in ensuring that all necessary documentation, including a sleep study confirming the diagnosis of sleep apnea, is included.
It's important to remember that Turnout is not a law firm and does not provide legal advice. However, they offer valuable support in navigating the claims process without needing legal representation. You're not alone in this journey, and we're here to help.
Obesity as a Secondary Condition to Sleep Apnea
Obesity can be a secondary condition, as it affects sleep quality. We understand that this connection is particularly relevant for veterans, many of whom may struggle due to various factors, including medication side effects.
It's common to feel overwhelmed. However, there are resources available. When seeking help, you should:
- Consult a healthcare provider, particularly a sleep specialist.
This can improve your overall health and well-being.
Remember, you are not alone. We're here to help you navigate your options.
Depression Linked to Sleep Apnea
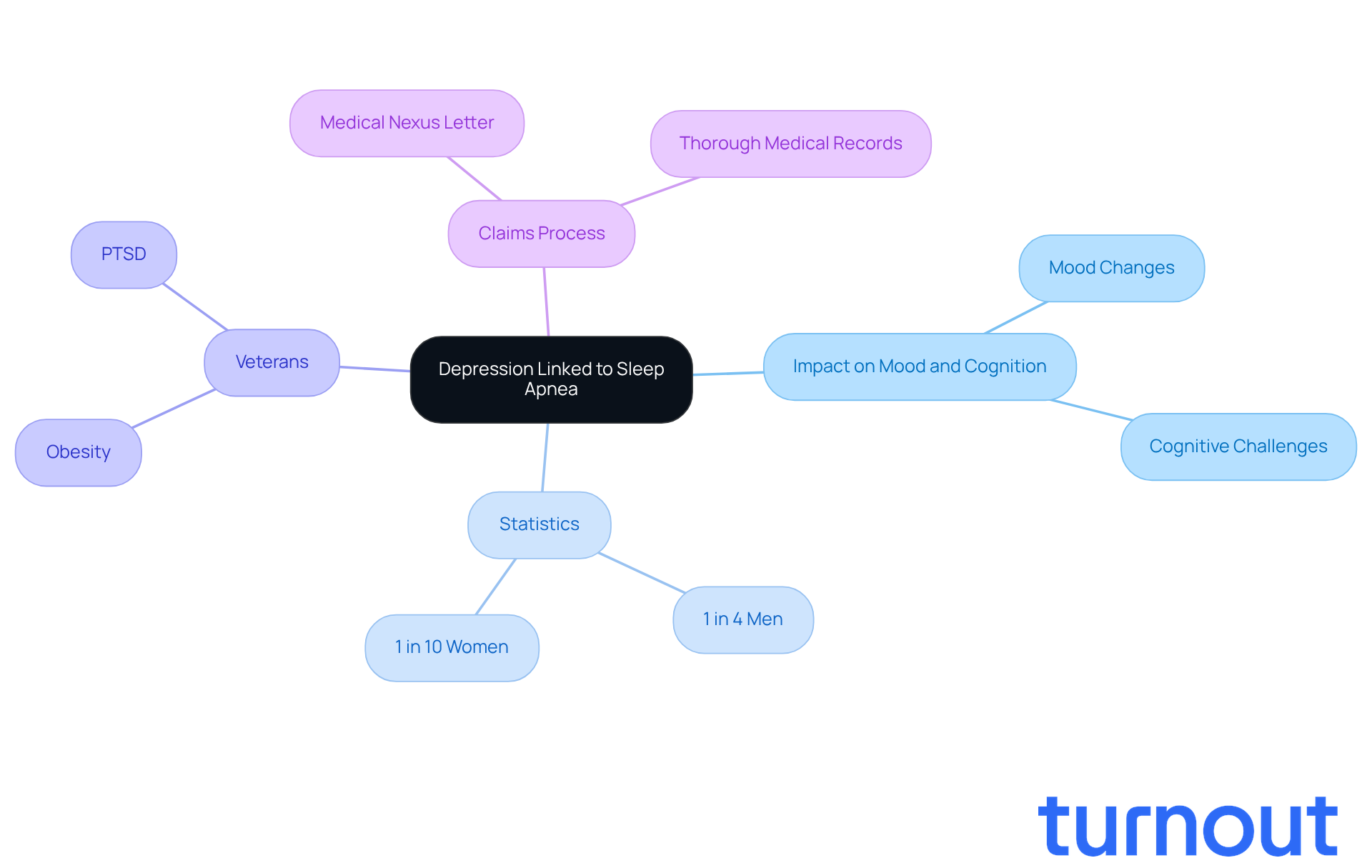
Depression often accompanies sleep apnea. We understand that these disturbances can lead to significant mental health issues. Research shows that sleep apnea not only triggers depression but can also exacerbate existing conditions.
For veterans, this connection is particularly important. Did you know that 1 in 5 veterans and 1 in 10 women in middle age experience depression? This issue is especially prevalent among veterans, often due to factors like obesity and PTSD. It’s crucial for veterans to ensure their requests accurately reflect this relationship, as it can significantly influence their claims and benefits.
The process to obtain support is essential. Acquiring a diagnosis that connects the two is vital for a successful claim. This letter should clearly outline how respiratory issues have contributed to or intensified the service member's depression. Remember, thorough documentation plays a key role in the claims process.
You are not alone in this journey. We’re here to help you and ensure you receive the support you need.
Understanding the Importance of Recognizing Secondary Conditions to Sleep Apnea
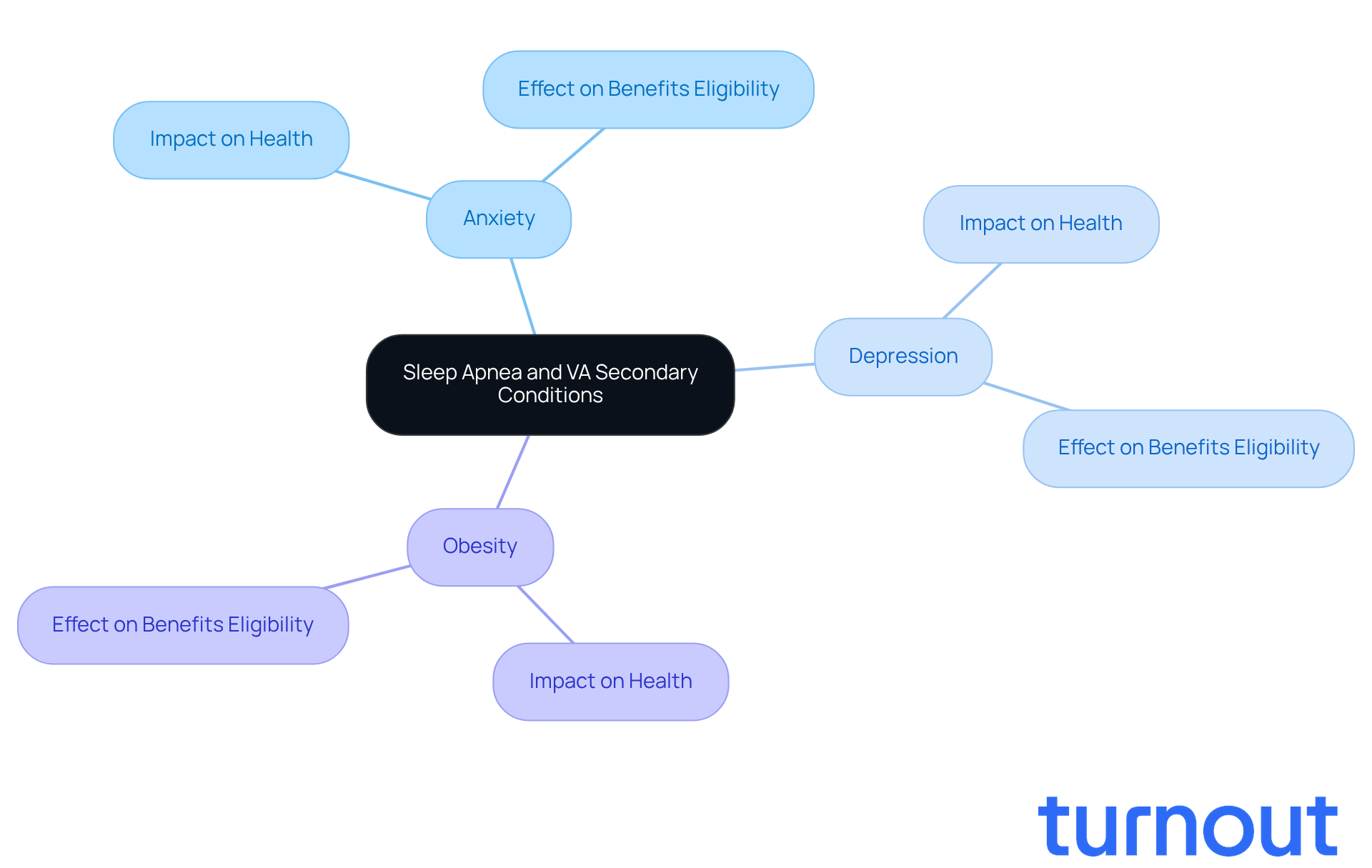
It is crucial for former military personnel seeking to identify conditions that are linked to sleep apnea. We understand that many veterans may not realize how secondary conditions can be considered intertwined with their breathing difficulties during rest. This connection can significantly impact their overall health.
Research shows that about 14% of adults with sleep apnea report experiencing anxiety. Additionally, obesity - a recognized risk factor for sleep apnea - continues to rise among former military personnel. It's common to feel overwhelmed by these challenges, but recognizing them is the first step toward better health.
Importantly, the VA can assess secondary conditions independently and include them in the total disability rating. This can enhance an individual's application and improve their chances of receiving the support they need. Comprehensive assessments and detailed records from healthcare providers are essential for navigating the compensation process effectively.
Veterans must demonstrate that their illness or injury is related to their service. Therefore, we encourage you to discuss all secondary conditions. This proactive approach can lead to a more accurate assessment of your conditions and ensure you receive the necessary support.
Understanding the relationship between sleep apnea and secondary conditions can strengthen a veteran's claim. By addressing these interconnected issues, you may find yourself on the path to increased benefits and an improved quality of life. Remember, you are not alone in this journey; we're here to help.
Conclusion
Understanding the connections between sleep apnea and various secondary conditions is crucial for veterans looking to enhance their health and secure the benefits they deserve. The relationships among conditions like:
- anxiety
- asthma
- PTSD
- GERD
- hypothyroidism
- tinnitus
- sinusitis
- obesity
- depression
show just how deeply sleep apnea can affect overall well-being. Recognizing these links can significantly impact a veteran's disability rating and access to essential support.
Throughout this article, we've shared key insights about how these secondary conditions aren't merely coexisting issues; they often intertwine with the challenges posed by sleep apnea. For example, anxiety and depression can worsen sleep disturbances, while conditions like asthma and GERD may be aggravated by interrupted breathing during sleep. Each of these relationships underscores the importance of thorough documentation and proactive communication with healthcare providers to strengthen claims for VA benefits.
Ultimately, addressing sleep apnea and its secondary conditions is about more than just navigating the claims process; it’s about enhancing quality of life. Veterans are encouraged to take action by discussing their symptoms with healthcare professionals and ensuring that all relevant health issues are documented. By understanding and advocating for these interconnected conditions, veterans can pave the way for better health outcomes and greater support from the VA. Remember, assistance is available, and you are not alone in this journey toward improved health and well-being.
Frequently Asked Questions
How is anxiety related to sleep apnea in veterans?
Anxiety disorders are common among veterans, particularly those experiencing breathing interruptions during sleep. This connection highlights how anxiety can exacerbate health issues related to sleep apnea.
Why is it important for veterans to recognize anxiety as a secondary condition to sleep apnea?
Recognizing anxiety as a secondary condition to sleep apnea is crucial for veterans seeking VA benefits, as it can potentially improve their disability rating.
What should veterans do to strengthen their claims for anxiety related to sleep apnea?
Veterans should gather comprehensive medical records from healthcare professionals that clearly link their anxiety to breathing disorders during rest, as this documentation can enhance their chances of receiving benefits.
What is the relationship between asthma and sleep apnea?
Asthma and nighttime breathing issues often co-occur, with breathing interruptions worsening asthma symptoms and increasing airway inflammation. Individuals with asthma face a higher risk of developing obstructive breathing issues.
How can veterans document the connection between asthma and sleep apnea for VA benefits?
Veterans need to provide thorough documentation of their asthma severity and its relationship to breathing interruptions during rest to establish VA secondary conditions to sleep apnea.
What role does a sleep study play in obtaining VA disability compensation for sleep disorders?
A sleep study is essential to confirm a diagnosis of a sleep disorder, which is necessary for VA disability compensation related to sleep apnea.
How does Post-Traumatic Stress Disorder (PTSD) relate to sleep apnea in veterans?
There is a significant connection between PTSD and breathing interruptions during sleep, where interrupted breathing can worsen PTSD symptoms, and PTSD distress can intensify breathing issues.
What percentage of individuals with PTSD also have sleep apnea as a secondary condition?
Over 57% of individuals diagnosed with PTSD also have VA secondary conditions to sleep apnea, highlighting the commonality of this dual diagnosis.
What documentation is needed for veterans to support their claims related to PTSD and sleep apnea?
Veterans should provide thorough documentation, including medical records, study results, and personal accounts, to strengthen their case for compensation related to PTSD and sleep apnea.
How can veterans get support in navigating claims related to sleep apnea and its secondary conditions?
Organizations like Turnout offer assistance through trained nonlawyer advocates who help veterans navigate the complexities of their SSD claims and ensure they receive the support they need.
List of Sources
- Anxiety as a Secondary Condition to Sleep Apnea
- Incidences of anxiety disorders among active duty service members between 1999 and 2018 (https://sciencedirect.com/science/article/abs/pii/S0887618522000810)
- Why VA pays more in disability for sleep apnea than it does for some lost limbs (https://washingtonpost.com/investigations/interactive/2025/va-disability-sleep-apnea-rating-payout)
- Sleep Disorders in US Military Personnel: A High Rate of Comorbid Insomnia and Obstructive Sleep Apnea - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC4694100)
- A Veteran's Journey to a Successful Claim - Linking Sleep Apnea to Service (https://vetlawoffice.com/blog/a-veterans-journey-to-a-successful-claim-linking-sleep-apnea-to-service)
- VA Sleep Apnea Ratings May Be Changing - Why Veterans Should File Now (https://portlanddisabilitylaw.com/va-sleep-apnea-ratings-may-be-changing-why-veterans-should-file-now)
- Asthma Linked to Sleep Apnea
- news.va.gov (https://news.va.gov/143430/va-research-wrap-up-ptsd-sleep-apnea-food)
- Why VA pays more in disability for sleep apnea than it does for some lost limbs (https://washingtonpost.com/investigations/interactive/2025/va-disability-sleep-apnea-rating-payout)
- Sleep Apnea Secondary to Asthma VA Disability Benefits | CCK Law (https://cck-law.com/blog/sleep-apnea-secondary-to-asthma)
- Understanding the Link Between Asthma and Obstructive Sleep Apnea in Veterans | Hill & Ponton, P.A. (https://hillandponton.com/obstructive-sleep-apnea-link-to-asthma)
- Post-Traumatic Stress Disorder as a Secondary Condition to Sleep Apnea
- news.va.gov (https://news.va.gov/143430/va-research-wrap-up-ptsd-sleep-apnea-food)
- Why VA pays more in disability for sleep apnea than it does for some lost limbs (https://washingtonpost.com/investigations/interactive/2025/va-disability-sleep-apnea-rating-payout)
- Sleep Apnea Secondary to PTSD: VA Disability Ratings & Benefits | CCK Law (https://cck-law.com/blog/sleep-apnea-secondary-ptsd-va-disability-benefits)
- Among Military With PTSD, Sleep Apnea Presents Hidden Threat | Psychiatric News (https://psychiatryonline.org/doi/full/10.1176/appi.pn.2023.12.11.9)
- Sleep Apnea Reported in 57% of Veterans with PTSD (https://respiratory-therapy.com/miscellaneous/sleep-apnea-reported-57-percent-veterans-ptsd)
- Gastroesophageal Reflux Disease (GERD) Secondary to Sleep Apnea
- VA Secondary Conditions to Sleep Apnea & Disability Benefits | CCK Law (https://cck-law.com/blog/va-secondary-conditions-to-sleep-apnea)
- Hypothyroidism as a Secondary Condition to Sleep Apnea
- Obstructive Sleep Apnea in Hypothyroidism - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC9850883)
- Frontiers | Association between hypothyroidism and obstructive sleep apnea: a bidirectional Mendelian randomization study combined with the geo database (https://frontiersin.org/journals/neurology/articles/10.3389/fneur.2024.1420391/full)
- VA Conditions Secondary to Sleep Apnea | Veterans Guide (https://veteransguide.org/conditions/secondary/sleep-apnea)
- Tinnitus Linked to Sleep Apnea
- Service Connecting Tinnitus and Sleep Apnea to Increase VA Rating - Veterans Disability Info (https://veteransdisabilityinfo.com/blog/service-connecting-tinnitus-and-sleep-apnea-to-increase-va-rating)
- VA Changes: Mental Health, Sleep Apnea & Tinnitus (2025 Update) CCK Law (https://cck-law.com/blog/2022-va-proposed-updates-mental-health-sleep-apnea-and-tinnitus)
- 2026 VA Rating Changes Explained: Key Updates and Potential Timelines for Veterans! (https://vaclaimsinsider.com/va-rating-changes-explained)
- Sinusitis as a Secondary Condition to Sleep Apnea
- VA Disability for Sleep Apnea Secondary to Sinusitis | CCK Law (https://cck-law.com/blog/va-disability-for-sleep-apnea-secondary-to-sinusitis)
- Obesity as a Secondary Condition to Sleep Apnea
- Why VA pays more in disability for sleep apnea than it does for some lost limbs (https://washingtonpost.com/investigations/interactive/2025/va-disability-sleep-apnea-rating-payout)
- Obesity and Sleep Apnea: Understanding the Connection (https://obesitymedicine.org/blog/sleep-apnea-and-obesity)
- Body weight and obstructive sleep apnea: a mathematical relationship between body mass index and apnea-hypopnea index in veterans - PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC9713905)
- Army Veteran joined MOVE! and lost 205 pounds - VA News (https://news.va.gov/140116/army-veteran-joined-move-lost-205-pounds)
- Sleep Apnea and Obesity (https://sleepapnea.org/sleep-health/obesity-and-sleep-apnea)
- Depression Linked to Sleep Apnea
- Better Sleep Improve Mental Health for Veterans (https://padentalsleep.com/better-sleep-improve-mental-health-for-veterans)
- Why VA pays more in disability for sleep apnea than it does for some lost limbs (https://washingtonpost.com/investigations/interactive/2025/va-disability-sleep-apnea-rating-payout)
- A Veteran's Journey to a Successful Claim - Linking Sleep Apnea to Service (https://vetlawoffice.com/blog/a-veterans-journey-to-a-successful-claim-linking-sleep-apnea-to-service)
- Is Depression Secondary to Sleep Apnea? - Veterans Disability Info (https://veteransdisabilityinfo.com/blog/is-depression-secondary-to-sleep-apnea)
- Understanding the Importance of Recognizing Secondary Conditions to Sleep Apnea
- Why VA pays more in disability for sleep apnea than it does for some lost limbs (https://washingtonpost.com/investigations/interactive/2025/va-disability-sleep-apnea-rating-payout)
- The VA’s disability evaluation is failing veterans (https://thehill.com/opinion/healthcare/5597999-va)
- VA Changes: Mental Health, Sleep Apnea & Tinnitus (2025 Update) CCK Law (https://cck-law.com/blog/2022-va-proposed-updates-mental-health-sleep-apnea-and-tinnitus)
- Veterans Often Overlook These VA Disability Claims: Secondary Conditions Explained (https://military.com/benefits/veterans-health-care/veterans-often-overlook-these-va-disability-claims-secondary-conditions-explained.html)
- VA Conditions Secondary to Sleep Apnea | Veterans Guide (https://veteransguide.org/conditions/secondary/sleep-apnea)




